

Background: Animal models have demonstrated that enthesitis is the primary lesion in experimental spondyloarthritis (SpA). In mice, innate lymphocytes were suggested as the major cytokine producers at the enthesis.
Objectives: We tested the hypothesis that the human enthesis harbours tissue resident conventional T-cells. We also assessed their ability to express SpA-related cytokines including TNF and IL-17A and if this could be blocked using psoriasis therapeutic agents (methotrexate (MTX), and phosphodiesterase type 4 inhibitor (PDE4i)) and experimental RORγt inhibitors (RORγti).
Methods: Entheseal spinous process was obtained from patients undergoing elective orthopedic procedures (n=20) and mechanically digested or processed for confocal staining and flow cytometry. CD4+ and CD8+ T-cells were sorted and RNA was isolated and analysed by qPCR. Magnetically isolated cells were stimulated using an anti-CD3/CD2/CD28 bead with and without the presence of MTX, RORγti and PDE4i. Following stimulation IL-17A and TNF were measured by ELISA and intracellular flow cytometry.
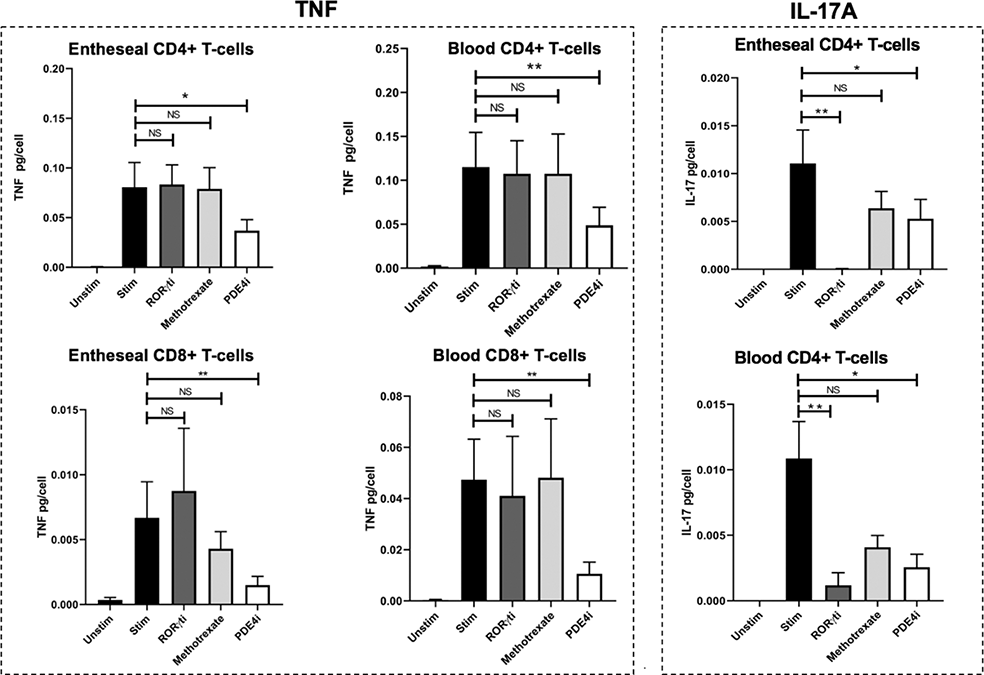
Results: CD4+ and CD8+ T-cells represent 35.7% and 23.7% of T-cells in the enthesis, respectively, with topographic confirmation by anti-CD3 immunofluorescence staining. Entheseal tissue contained a higher proportion of CD4+ and CD8+ T-cells expressing a resident memory phenotype (CD69+/CD45RA-) compared to matched blood. Sorted T-cells from entheseal tissue had a gene expression profile consistent with a tissue resident phenotype and CD4+ and CD8+ T-cells showed increased expression immunomodulatory genes including IL-10 and TGF-β compared to peripheral blood T-cells (p<0.001). Following stimulation CD4+ T-cells produced more TNF than CD8+ T-cells (p<0.05), IL-17A was robustly detected in CD4+ but not CD8+ T-cells. TNF and IL-17A production from CD4+ T-cells was effectively inhibited by PDE4i (p<0.05), while RORγti only reduced IL-17 secretion (p<0.001). MTX had no significant impact on both TNF and IL-17A production in either cell population. This pattern of inhibition was mirrored in TNF secretion from CD8+ T-cells.
Conclusion: This is the first description of conventional CD4+ and CD8+ enthesis resident T-cells. PDE4i was effective in abrogating induced TNF production and IL-17, whereas RORγti is highly effective for IL-17A production but not TNF. In contrast, MTX had little effect on in vitro enthesitis model cytokine production. These findings may have some practical implications in the treatment of subclinical enthesitis.
Effect of different therapeutic agents on the TNF and IL-17A production by resident entheseasl T -cells and matched peripheral blood
Gene expression profile of entheseal T-cells (soft tissue and adjacent bone) compared to peripheral blood
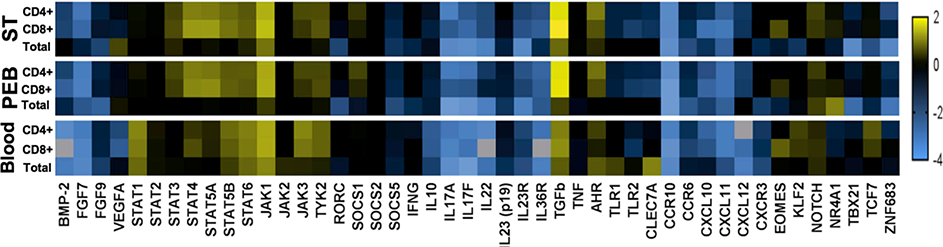
Abbreviations: ST, entheseal soft tissue; PEB, peri-entheseal bone.
Disclosure of Interests: Abdulla Watad: None declared, Hannah Rowe: None declared, Charlie Bridgewood: None declared, Tobias Russell Grant/research support from: PhD Project is funded by Novartis., Qiao Zhou: None declared, Almas Khan: None declared, Robert Dunsmuir: None declared, Peter Loughenbury: None declared, Abhay S Rao: None declared, Peter Millner: None declared, Richard Cuthbert: None declared, Dennis McGonagle Consultant for: Lilly, Novartis UCB, Speakers bureau: Lilly, Novartis UCB
DOI: 10.1136/annrheumdis-2019-eular.1087