

Background: Psoriatic arthritis (PsA) is a chronic inflammatory joint disease typically associated with psoriasis and classified in the group of spondyloarthritis (1). The pathogenesis is based on an interplay of different genes interacting with several environmental factors including stress, trauma, infections, triggering an inflammatory response related to the activation of innate and acquired immunity in different tissues and organs (2). However, the risk for the development of PsA is not clearly understood.
Objectives: The aim of this study was to evaluate, in a cohort of Italian PsA out-patients of the Rheumatology Unit of the University of Rome Tor Vergata, the association of genetic variants in candidate genes for PSA susceptibility and their possible contribute in the modulation of clinical and laboratory features.
Methods: The genes were selected according to previous studies describing these genes as involved in susceptibility to rheumatoid arthritis (RA) (3), since a common genetic background can be shared between these diseases. Nine SNPs (single nucleotide polymorphism) in eight candidate genes were analysed: STAT4 (rs7574865), TRAF3IP2 (rs33980500), TNFAIP3 (rs6920220 and rs2230926), MIR146A (rs2910164), PSORS1C1 (rs2233945), IL-10 (rs1800872), HCP5 (rs3099844) and ERAP1 (rs27524). Polymorphisms were analysed in 163 consecutive PsA out-patients and 198 healthy controls (HC). Genotyping was performed by allelic discrimination by TaqMan assay. Alleles frequencies differences between cases and controls or between phenotypic groups were compared using Pearson’s χ 2 test.
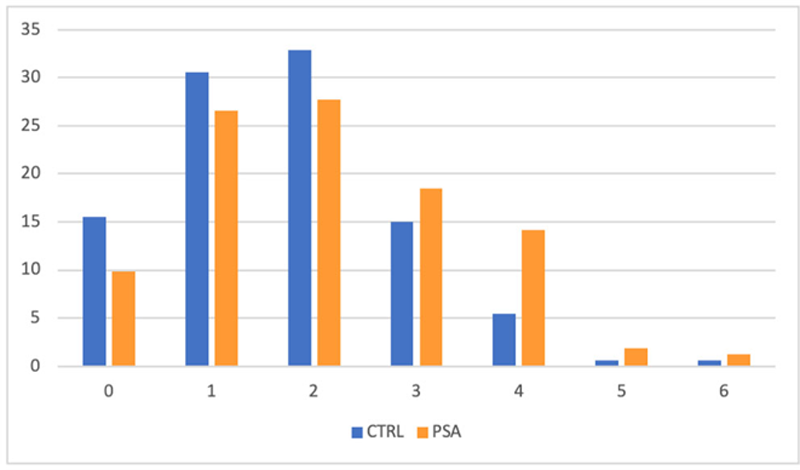
Results: We have observed an association between PSA susceptibility and the variant alleles of STAT4 [OR= 1.60 (1.15-2.21), P= 0.005], TRAF3IP2 [OR= 1.65 (1.01-2.65), P= 0.04], ERAP1 [OR= 1.40 (1.05-1.85), P= 0.02] and TNFAIP3 (rs6920220) [OR= 1.75 (1.19-2.57), P= 0.004]. On the contrary, the variant allele of IL-10 polymorphism seems to play a protective role [OR= 0.74 (1.05-1.85), P= 0.05]. Moreover, in order to define a genetic risk profile, we have counted the total number of risk alleles in each subject, considering as risk alleles the allelic variant of rs7574865 (STAT4), rs33980500 (TRAF3IP2), rs6920220 (TNFAIP3) and rs27524 (ERAP1) SNPs. Then, we have compared the risk allele number distribution between patients and HC (
Number of risk alleles in patients and controls: rs7574865 (STAT4), rs33980500 (TRAF3IP2), rs6920220 (TNFAIP3) and rs27524 (ERAP1) SNPs.
Conclusion: We confirm the associations between five SNPs, already studied in RA, and PSA susceptibility, suggesting a common inflammatory pathway in chronic inflammatory rheumatological diseases. Moreover, we show how the genotyping of only few associated SNPs could help to define a genetic risk profile for PSA development.
REFERENCES:
[1]Calabresi E, et al. One year in review 2019: psoriatic arthritis. Clin Exp Rheumatol. 2020;38:1046-55.
[2]Chimenti MS, Triggianese P, De Martino E, Conigliaro P, Fonti GL, Sunzini F, Caso F, Perricone C, Costa L, Perricone R. An update on pathogenesis of psoriatic arthritis and potential therapeutic targets. Expert Rev Clin Immunol. 2019 Aug;15(8):823-836.
[3]Ciccacci C, et al. Polymorphisms in STAT-4, IL-10, PSORS1C1, PTPN2 and MIR146A genes are associated differently with prognostic factors in Italian patients affected by rheumatoid arthritis. Clin Exp Immunol. 2016;186:157-63.
Disclosure of Interests: None declared