

Background: Pulmonary interstitial disease(ILD)is very common in connective tissue disease (CTD). Different subtypes display significant differentiations in prognosis. Pirfenidone (PFD), the targeted anti-fibrosis and anti-inflammatory drug, started to apply in CTD-ILD, while its strategy of combination with immunotherapy, bridging time and service time are worth discussing.
Objectives: To evaluate the efficacy and safety of PFD combined with immunosuppressant (IS) in the treatment of several CTD- ILD.
Methods: 111 CTD-ILD patients were involved from Aug 2019 to Dec 2021 (ClinicalTrials.gov Identifier NCT04928586), including systemic sclerosis (SSc, n=30), inflammatory myopathy (IIM, n=51), rheumatoid arthritis (RA, n=17) and other CTDs (such as systemic lupus erythematosus, sjogren’s syndrome, n=13). Patients were treated with relative stable dose of glucocorticoid (GC) and/or IS since screening.After the evaluation of HRCT, pulmonary function (FVC% and DLCo%) and basic disease activity, PFD was added or not and followed up regularly for 24 weeks. The changes of lung function and imaging were recorded in different subgroups.
Results: At baseline, The FVC% in the SSc-PFD (n=14), IIM-PFD (n=25) pts were lower than that of SSc-no-PFD (n=16), IIM-no-PFD (n=26) respectively, that was 81.06 vs 99.63( p = 0.014), 78.23 vs 91.12, ( p = 0.010). And IIM-PFD group present a lower baseline DLCo% than IIM-no-PFD pts (64.25 vs 72.82, p =0.034). DLCo% in the other CTDs was lower than SSc, IIM, RA pts (54.58 vs 65.55, 68.71, 66.89, p =0.036), while there were no significant differences in baseline FVC% among these disease.
After 24 weeks of treatment, FVC% in SSc-PFD group was improved by 7.15%, while that was -0.91% in SSc-no-PFD pts (
p
=0.042). The elevation in FVC% was also significant between the IIM-PFD and IIM-no-PFD control (8.00
vs
1.40,
p
=0.016). On the other hand, DLCo% of RA-PFD obviously enhanced 7.40%, compared with RA-no-PFD decrease 5.50% from baseline(
p
=0.002) (
The changes of FVC% and DLco% in PFD treated CTD-ILD for 24 weeks. (A ) FVC% changes in SSc, IIM, RA and other CTD-ILD from baseline.; (B ) DLco% changes in SSc, IIM, RA and other CTD-ILD from baseline. * p < 0.05, compared to no PFD treatment group.
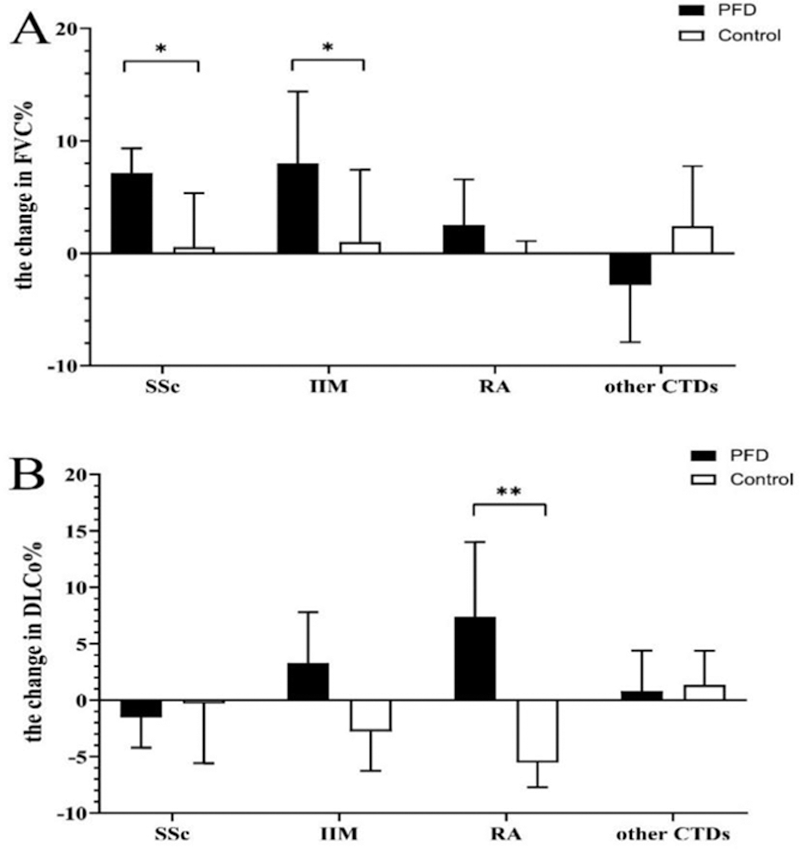
When performing subgroup analysis with manifestations in HRCT, the change of FVC% in SSc-PFD pts with usual interstitial pueumonia tendency(SSc-PFD-UIP) was higher than SSc-PFD-non-UIP group (8.05 vs -3.20, p =0.014). However, the non-UIP tendency in IIM-PDF pts displayed superior therapeutic effects than IIM-PDF-UIP pts (10.50 vs 1.00, p =0.005). In addition, DLCo% improved significantly in RA-PDF-non-UIP subgroup, compared with RA-PDF-UIP pts (10.40 vs -4.45, p =0.017).
According to whether the baseline FVC% and DLCo% value was less than 70%, the improvement of FVC% was significantly higher in PFD treatment group than no-PFD pts of SSc and IIM with baseline High-FVC%(6.60 vs 0.10, p =0.047),(6.30 vs 1.10, p = 0.089).In RA-PFD pts, DLCo% showed a significant increase in baseline DLCo% less than 70% subgroup, compared to RA-no-PDF (7.40% vs -6.60%, p=0.011).The basic IS were considerable between PFD andno-PFD pts throughout the study and no differences of GS and IS dosages at baseline and follow up among all subgroups.
Multiple linear regression analysis found that baseline FVC%<70%(HR=4.56,6.81) and prescription of PFD(HR=4.56,4.37) could positively affect the changes of FVC% and DLCo% (all p <0.05).
Conclusion: The response of pulmonary function to PFD were varied in different CTD-ILD subsets. SSc and IIM pts acquired obviously improvement on FVC%, especially with high baseline FVC group. DLco% elevated in RA-PFD, highlight those baseline Low-DLco and No-UIP pts.
Acknowledgements: Funded by ECCM Program of Clinical Research Center of Shandong University (No. 2021SDUCRCB010)
Disclosure of Interests: None declared