

Background Systemic lupus erythematosus (SLE) is a multisystemic autoimmune disease with several aberrancies in the immune system[1]. Genetics factors are central to understanding the pathophysiology especially in patients with monogenic lupus (single-gene mutation)[2]. Anecdotally, we observe a relatively high prevalence of familial SLE in our region (UAE/Arab regions). Studying the genetics of such cases have yielded gene mutations known to cause SLE. Here we report 3 siblings with mutations in DNAES1L3 causing SLE and hypocomplementenemic urticarial vasculitis (HUVS)[3].
Objectives To report the clinical and genetic presentation of 3 siblings with monogenic SLE and HUVS and discuss clinicopathologic correlations.
Methods The patients were identified through our SLE clinical cohort. Informed consent was obtained from the patients/guardians to participate in our institution’s “Mendelian Project” research study. The study is approved by the local IRB committee. Whole exome sequencing (WES) was performed. The results of the initial sequencing were analyzed in the context of the clinical presentation of SLE and HUVS.
Results Genetic analysis via WES revealed a homozygous DNASE1L3 variant at c.572A>G; p. Asn191Ser for the 3 affected siblings classified as variant of unknow significance (VUS). The mother and healthy sibling were heterozygous (carrier) for the variant. This indicate that the variant is segregating with the family for SLE. DNASE1L3 variant c.572A>G, p.Asn191Ser is a novel variant that was not reported previously in the literature or human genetic mutation database (HGMD). Computational (in-silico) pathogenicity prediction tools predicted damaging effect of the variant (PolyPhen: damaging, SIFT: Deleterious, Conservation: high). Clinical and laboratory features are presented in Table 1. All three siblings developed HUVS as the initial manifestation which was confirmed by skin biopsy. In the older siblings who eventually met the criteria for SLE, the HUVS resolved as other SLE symptoms emerged. The youngest sibling has not met criteria for SLE and only has skin involvement with debilitating HUVS (tender lesions and swollen hands/feet). This patient was found to have very low levels of C1q without anti-C1q antibodies. Screening for mutations in C1q was negative. Of note, the HUVS has been the most severe in this patient.
| Patient 1 | Patient 2 | Patient 3 | |
|---|---|---|---|
| Age at onset | 13 months | 2 years | 3 years |
| Age at SLE diagnosis | N/A | 6 years | 3 years |
| Current age | 2 years | 7 years | 17 years |
| Clinical findings | |||
| HUVS | +# | + | +# |
| Fever | + | + | + |
| Lymphadenopathy | + | + | - |
| Arthritis | - | - | - |
| Mucocutaneous ulcers | - | - | - |
| Glomerulonephritis | - | Class II/V | Class IV |
| Lab findings | |||
| Positive ANA | - | + | + |
| Positive anti-dsDNA | - | + | + |
| Low C3/low C4 | +/- | +/- | +/+ |
| Low C1q/anti-C1q antibodies | +/-$ | NA/NA | NA/NA |
| ↓Hgb/↓WBC/↓plt | +/-/- | -/+/- | +/-/- |
| ↓ IgG | - | - | + |
| Positive aPLs | - | - | - |
# HUVS confirmed by skin biopsy. $ Mutation in C1q gene not detected.
Conclusion DNASE1L3 genetic variants contribute to monogenic SLE. This report supports prior literature linking DNAES1L3 deficiency to HUVS in addition to SLE. Further analysis of the effect of this variant on the immune system and link to C1q deficiency or consumption may shed light on relevant immune mechanisms related to SLE.
References
Image/graph:
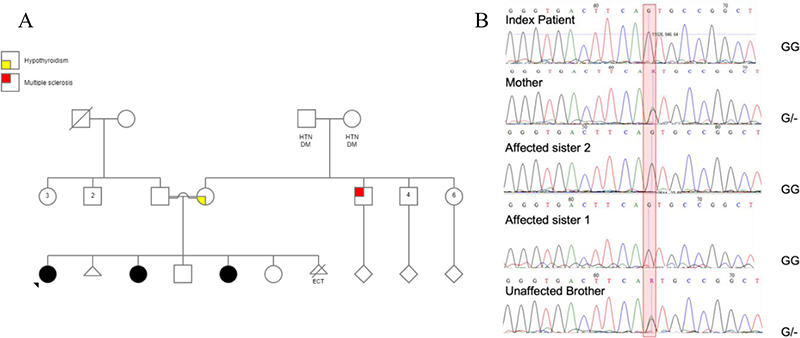
Figure 1. A. Family pedigree of index case (youngest sibling) with DNASE1L3 (c.572A>G, p.Asn191Ser). B. A segregation analysis of DNASE1L3 gene variant c.572A>G, p.Asn191Ser for the family members. The red bar highlighting the genotype of the patients and family members.
Acknowledgements: NIL.
Disclosure of Interests None Declared.
Keywords: Systemic lupus erythematosus, Genetics/Epigenetics
DOI: 10.1136/annrheumdis-2023-eular.1626