

Background TelessaúdeRS-UFRGS is a university-based telemedicine project in Brazil that receives support and resources from Brazil’s Ministry of Health, and the State Health Department of Rio Grande do Sul. Since 2013, TelessaúdeRS has provided a synchronous toll-free telephone teleconsulting service that supports primary health care (PHC) physicians across the country. Family medicine, internal medicine, and rheumatology specialists answer clinical inquiries using the best evidence. (1)
Objectives Describe the prevalence of specific rheumatology topics, recommendations provided in teleconsultations, and the change in the utilization pattern of this service over time.
Methods In this cross-sectional study, we retrospectively extracted data from the TelessaúdeRS-UFRGS database. Teleconsultations were included from September 21, 2018, to January 25, 2022, addressing rheumatologic topics. Teleconsultations with incomplete data were excluded. Teleconsulting involves the discussion of clinical cases between patients’ physicians and a rheumatologist or a trained PHC physician. All teleconsultations are registered in the TelessaúdeRS-UFRGS database. The teleconsultant formulates a diagnostic hypothesis, and a decision (based on referral protocols) is taken: referral to rheumatology, emergency care, stay in PHC or re-evaluation after a treatment course, or diagnostic tests. Criteria for referral to a rheumatologist were: diagnosis or high suspicion of systemic inflammatory disease, diagnosis still in doubt after re-evaluation, or non-inflammatory rheumatic diseases refractory to treatment. Besides the consultant’s recommendation, the assistant doctor has the final decision about the referral. Chi-square test was used for statistical analysis.
Results A total of 7715 teleconsultations were eligible for analysis after excluding 39 cases with incomplete data. The most frequent diagnostic hypotheses generated during teleconsultations were rheumatoid arthritis (RA), non-specific arthralgia/arthritis, and systemic lupus erythematosus (Table 1). Fibromyalgia, gout, and osteoarthritis were other diagnostic hypotheses commonly considered. Almost one-third (n=2219; 29% of total consultations) of the discussions referred to patients already waiting for rheumatology consultation, and teleconsulting replaced the in-person specialist evaluation in 32% (n=722) of these cases. Of the 5496 that were not waitlisted, 1369 (24.9%) were referred after teleconsulting. In total, 54.9% of the teleconsultations decided that the patients could be adequately managed in the PHC. The Figure 1 describes the utilization pattern of the rheumatology teleconsulting service during the time frame of this study. The utilization of the teleconsulting service increased significantly, and the proportion of patients referred to in-person rheumatology consultations reduced over the last years (P<0.001).
| Diagnostic hypotheses formulated after teleconsulting, n=7715 (%) | |
|---|---|
| Rheumatoid arthritis | 1665 (21.6%) |
| Undifferentiated arthralgia/arthritis | 1298 (16.8%) |
| Systemic lupus erythematosus | 830 (10.8%) |
| Fibromyalgia | 570 (7.4%) |
| Laboratory test | 547 (7%) |
| Gout | 466 (6%) |
| Spondylarthritis | 432 (5.6%) |
| Osteoarthritis | 326 (4.2%) |
| Other connective tissue disease | 431 (5.6%) |
| Other soft tissue diseases | 396 (4.5%) |
| Osteoporosis | 153 (1.9%) |
| Others | 601 (7,7%) |
Figure 1.
Image/graph:
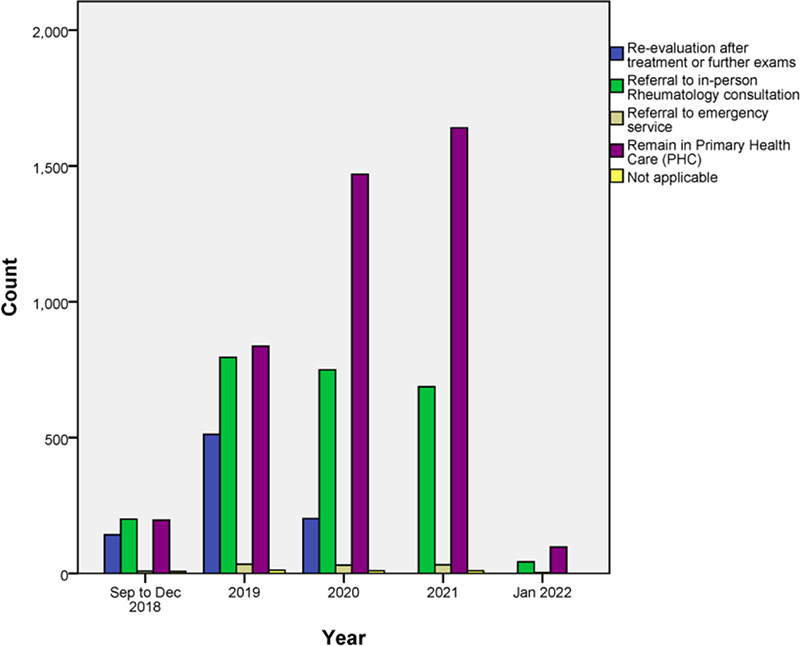
Conclusion Prevalent rheumatic diseases, especially RA, are frequent reasons for using teleconsulting support in our country. According to our study, after guidance, the PHC physician was considered able to manage most cases in rheumatology. This reduced the waiting list by approximately one-third. There was a progressive increase in teleconsultations over the years, but the proportion of patients referred to rheumatology reduced over time.
Reference [1] Gonçalves MR, et al. Ann Fam Med. 2017;15(4):383.
Acknowledgements: NIL.
Disclosure of Interests None Declared.
Keywords: Telemedicine, Quality of care, Health services research
DOI: 10.1136/annrheumdis-2023-eular.5275