

Background Sex hormones have effects on the development, progression and severity of SLE, prevalently affecting women (F:M=9:1). The neuroprotective, neurotrophic and anti-inflammatory properties of a class of progesterone-derived NeuroActive Steroids (NASs), prompted numerous investigations about the potential of these GABAA receptor allosteric modulators. However, no data about NASs on neuropsychiatric SLE (NPSLE) are available.
Objectives This exploratory pilot study aims to delve into a new unexplored landscape by assessing circulating NASs levels in NPSLE patients.
Methods A cohort of 16 SLE patients without NP manifestations and 16 with new onset NP diffuse symptoms was enrolled. Mood disorders and cognitive dysfunction were defined according to the Center for Epidemiologic Studies Depression Scale (CES-D) and a battery of neuropsychological tests, respectively, interpreted by a neuropsychologist. A group of 8 healthy controls (HCs) matched for mean age and gender ratio was also recruited. Exclusion criteria: ongoing contraceptive or hormonal treatment; glucocorticoid pulse or treatment variations 6-month before blood collection; anxiolitic, anticonvulsivant, antiepilettic drug intake; gonadal-adrenal surgical intervention or pathologies. Data regarding demographics, SLEDAI andSLICC organ damage index (SDI) were collected. NASs serum levels and their precursor were measured by ELISA assay, as listed: Progesterone, Diidroepiandrosterone (DHEA), Diidroepiandrosterone-Sulphate (DHEA-S), Allopregnanolone. To appreciate differences between groups, women’s fertile or menopausal subgroups were formed and p-value <0.05 has been set.
Results Table 1 reports on data from the whole cohort. Progesterone levels in fertile women were significantly higher in the NPSLE versus HCs group (p=0.011). The Progesterone-direct metabolite, Allopregnanolone, was significantly increased in NPSLE compared to both groups of fertile SLE (p=0.026) and HCs females (p=0.027). Inversely, low levels of DHEA and DHEA-S in SLE patients versus HCs (p=0.025 and p=0.005) were found. Looking for NP symptoms, DHEA titer inversely correlates with cognitive deficit diagnosis (p=0.04), while depression diagnosis (62.5% of NPSLE cohort) correlates with Allopregnanolone levels (p=0.042). Moreover, depression severity measured by the CES-D score correlates with Progesterone (r=0.550, p=0.041) and Allopregnanolone (r=0.712, p=0.004; Figure 1). At multivariate analysis after correction for age, disease duration, SLEDAI and SDI, Allopregnanolone confirmed its independent correlation (β=0.712, p=0.004) with depression severity.
Conclusion In this pilot study, we describe for the first time the unbalanced levels of the most potent neuroactive steroid Allopregnanolone in SLE fertile patients with new onset neuropsychiatric diffuse manifestations. Moreover, in NPSLE patients, the diagnosis of cognitive deficit associates with circulating DHEA low levels and that of depression associates with Allopregnanolone high levels, significantly correlated also with the severity of this manifestation. Since the appropriate NASs balance is needed for optimal brain and neuroimmune function, our preliminary observations – that needs to be validated in an extended cohort - open a new perspective in the field, where the circulating NASs assessment in NPSLE patient could be a new promising diagnostic and preclinical research strategy.
| NPSLE (16) | SLE (16) | HC (8) | |
|---|---|---|---|
| Age mean (DS) | 48.2 (15.9) | 42.1 (10.8) | 49 (16) |
| Gender (F, %) | 100 | 100 | 100 |
| Fertile (%) | 50 | 50 | 50 |
| Menopausal (%) | 50 | 50 | 50 |
| Disease duration, yrs median (IQR) | 6(2.3-9.3) | 6.7(3.0-10.4) | - |
| SLEDAI median (IQR) | 5 (1.8-11) | 2 (0-4) | - |
| Dose PDN mg/daily median (IQR) | 9.5 (5.1-14.6) | 3.8 (3.2-7) | - |
| Cognitive disorder (%) | 50 | - | - |
| Major depression (%) | 62.5 | - | - |
Image/graph:
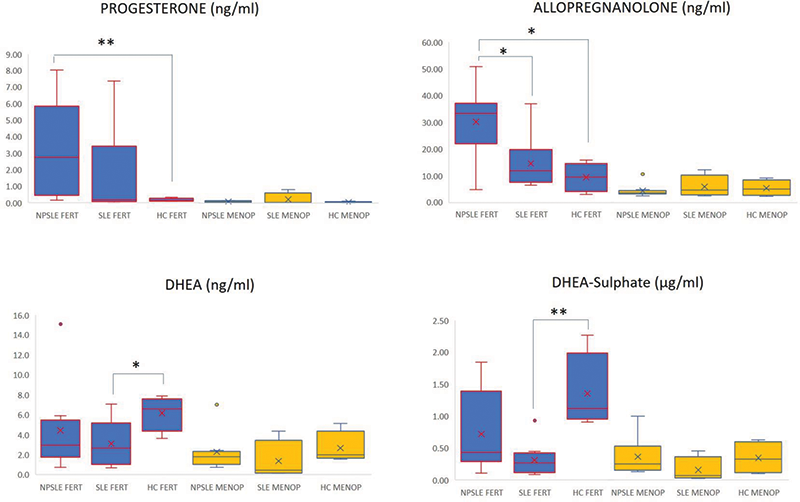
Figure 1. Median value of NASs circulating levels on NPSLE/SLE/HCs fertile and menopausal female. *pvalue ≤ 0,05; ** pvalue ≤ 0,01
Acknowledgements All staff of the Rheumatology Unit of the AOU of Cagliari, patients and volunteer donors.
Disclosure of Interests Maria Maddalena Angioni: None declared, Elisabetta Chessa: None declared, alessandra perra: None declared, elisa pintus: None declared, Alberto Floris: None declared, MATTIA CONGIA: None declared, Mauro Giovanni Carta: None declared, Alberto Cauli: None declared, Matteo Piga Speakers bureau: GSK, Consultant of: GSK, GALAPAGOS, ASTRAZENECA.
Keywords: Gender/diversity issues, Systemic lupus erythematosus, Mental health
DOI: 10.1136/annrheumdis-2023-eular.1993