

Background Anti-Ro60 and anti-Ro52 antibodies are associated with different connective tissue diseases (CTDs) [1]. However, the clinical significance of anti-Ro antibodies is not always consistent among different global regions.
Objectives To investigate the clinical characteristics of patients with anti-Ro antibodies.
Methods A total of 1596 inpatients with anti-Ro antibodies were included in the study. Demographic, clinical, and serological data were compared between individuals with different profiles of anti-Ro antibodies: patients with anti-Ro52 antibodies alone, patients with anti-Ro60 antibodies alone, and patients with combined anti-Ro52 and anti-Ro60 antibodies.
Results Of the 1596 patients, 1362 (85.3%) were female, the mean age was 45.5 years, and systemic lupus erythematosus (SLE) (46.0%) and Sjogren’s syndrome (SS) (19.0%) were the most common CTD diagnoses. Among the patients with anti-Ro52 antibodies alone, idiopathic inflammatory myopathy (18.8%) and SLE (17.6%) were the most common CTD diagnoses. The coexistent autoantibodies of this group were significantly lower compared with those of the other two groups, while the presence of anti-Jo1 antibodies were significantly higher compared with those of the other two groups (3.7% vs. 0.6% vs. 1.9%, p=0.029) (Figure 1). In addition, the patients with isolated anti-Ro52 antibodies were more likely to suffer from interstitial lung disease (35.5% vs.11.3% vs.13.7%, p<0.0001) and pulmonary arterial hypertension (10.1% vs. 5.3% vs. 3.6%, p=0.001) compared with the other two groups of patients (Table 1). Compared with patients with isolated anti-Ro52 or anti-Ro60 antibodies, the patients with combined anti-Ro52 and anti-Ro60 antibodies were more likely to suffer from xerophthalmia and xerostomia. Furthermore, hypocomplementemia, hyperglobulinemia, and proteinuria were particularly prevalent in patients with anti-Ro60 antibodies.
Conclusion Different profiles of anti-Ro antibodies were significantly associated with clinical phenotypic features in CTDs, indicating the potential diagnostic and prognostic value of these antibodies in clinical practice.
Reference [1]Lee A Y S, J H Reed, and T P Gordon. Anti-Ro60 and anti-Ro52/TRIM21: Two distinct autoantibodies in systemic autoimmune diseases. J Autoimmun, 2021 Nov;124:102724.
Image/graph:
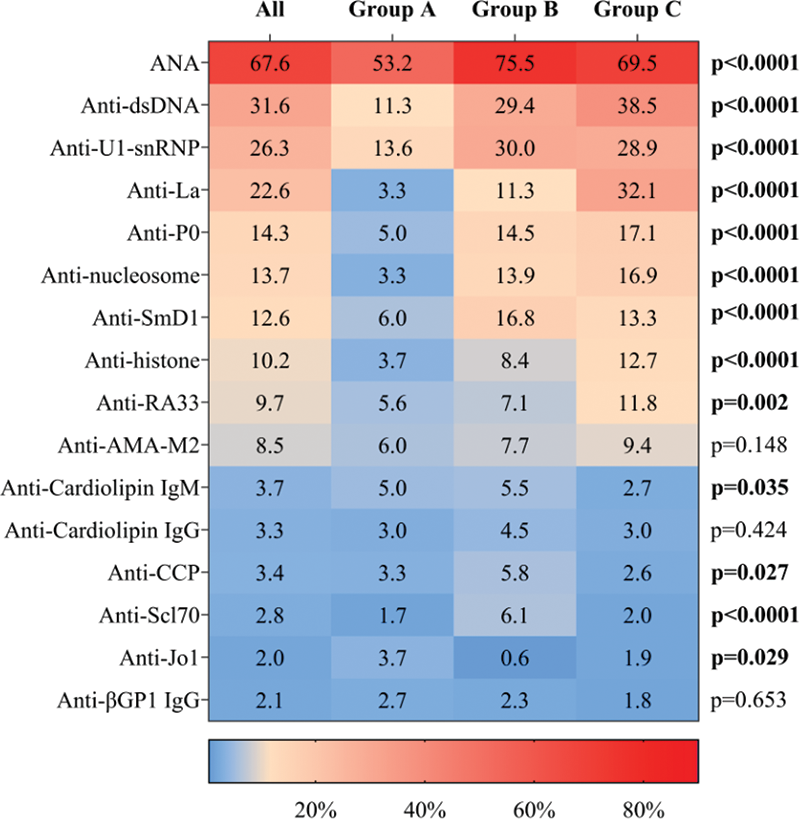
Figure 1 Comparison of autoantibody profiles in patients with positive anti-Ro antibodies
| Parameters (n, %) | Groups | p values | ||||||
|---|---|---|---|---|---|---|---|---|
| All: n=1319 | Group A: Ro52 alone n=169 | Group B: Ro60 alone n=283 | Group C: Ro60 and Ro52 n=867 | Group A vs. group B | Group A vs. group C | Group B vs. group C | Overall | |
| Skin rash | 349(26.5) | 40(23.7) | 101(35.7) | 208(24.0) | 0.008 | 0.928 | <0.0001 | <0.0001 |
| Arthralgia | 512(38.8) | 72(42.6) | 164(58.0) | 276(31.8) | 0.002 | 0.007 | <0.0001 | <0.0001 |
| Myalgia | 80(6.1) | 16(9.5) | 26(9.2) | 38(4.4) | 0.921 | 0.007 | 0.002 | 0.002 |
| Xerophthalmia | 277(21.0) | 31(18.3) | 39(13.8) | 207(23.9) | 0.160 | 0.118 | <0.0001 | 0.001 |
| Xerostomia | 310(23.5) | 34(20.1) | 47(16.6) | 229(26.4) | 0.346 | 0.085 | 0.001 | 0.002 |
| Anemia | 375(28.4) | 39(23.1) | 78(27.6) | 258(29.8) | 0.292 | 0.079 | 0.481 | 0.198 |
| Leukocytopenia | 295(22.4) | 28(16.6) | 61(21.6) | 206(23.8) | 0.197 | 0.041 | 0.446 | 0.114 |
| Thrombocytopenia | 128(9.7) | 11(6.5) | 27(9.5) | 90(10.4) | 0.261 | 0.121 | 0.685 | 0.297 |
| Proteinuria | 208(15.8) | 10(5.9) | 53(18.7) | 145(16.7) | <0.0001 | <0.0001 | 0.438 | 0.001 |
| Hematuria | 99(7.5) | 3(1.8) | 29(10.2) | 67(7.7) | 0.001 | 0.005 | 0.183 | 0.004 |
| ILD | 211(16.0) | 60(35.5) | 32(11.3) | 119(13.7) | <0.0001 | <0.0001 | 0.296 | <0.0001 |
| PAH | 63(4.8) | 17(10.1) | 15(5.3) | 31(3.6) | 0.056 | <0.0001 | 0.199 | 0.001 |
| RP | 88(6.7) | 18(10.7) | 22(7.8) | 48(5.5) | 0.297 | 0.013 | 0.172 | 0.036 |
ILD: interstitial lung disease; PAH: pulmonary arterial hypertension; RP: Raynaud’s phenomenon
Acknowledgements: NIL.
Disclosure of Interests None Declared.
Keywords: Autoantibodies, Clinical trials, Organ damage
DOI: 10.1136/annrheumdis-2023-eular.639