

Background Systemic lupus erythematosus (SLE) is an autoimmune disease of unknown etiology that can affect various organ systems, particularly the kidneys [1]. Interleukin-6 (IL-6), Interleukin-17 (IL-17), and tumour necrosis factor-α (TNF-α) are closely correlated with the risk of SLE and play a significant role in the pathogenesis of the disease. However, the causal relationship between these cytokines and the risk of SLE has not been elucidated.
Objectives Our study aimed to assess the causal association between the cytokines IL-17, IL-6, TNF-α, and SLE by Mendelian randomization (MR) study.
Methods Data on both cytokines and SLE were obtained from aggregate-level data from the publicly available Genome-Wide Association Study (GWAS), a Finnish database comprising mainly participants of European ancestry [2-3]. Bi-directional two-sample MR was performed using inverse variance weighting (IVW), MR-Egger regression and weighted median methods. In addition, MR-Egger regression and leave-one-out analyses were performed to assess the potential pleiotropy of these cytokines. Finally, the direct causal relationships between IL-17, IL-6 and TNF-α and SLE were estimated by multivariate MR analysis (MVMR).
Results The IVW results and MVMR analysis showed that IL-17 had a direct causal association with the risk of developing SLE (95% CI = 0.168~ 1.207, P = 0.009). No significant associations were observed between SLE and IL-6 (95%CI=-0.610-0.188, P=0.302) as well as TNF-α (95%CI=-0.120~0.178, P=0.707). Evidence from bidirectional MR did not support reverse causality. Specifically, the IVW results are as follows, IL-6 (OR=1.017, P=0.081), IL-17 (OR=1.015, P=0.122), and TNF-α (OR=1.027, P=0.063). Cochran’s Q test showed that there was no heterogeneity between these SNPs as IVs. Furthermore, the pooled causal effects from the MR-Egger regression analysis corroborated the IVW results, suggesting no significant heterogeneity across estimates of the included SNPs.
Conclusion In conclusion, the present study supports the hypothesis that genetically predicted higher levels of circulating IL-17 were directly associated with an increased risk of SLE. Accordingly, drugs targeting IL-17 may be highly effective and promising therapeutic options.
References
Image/graph:
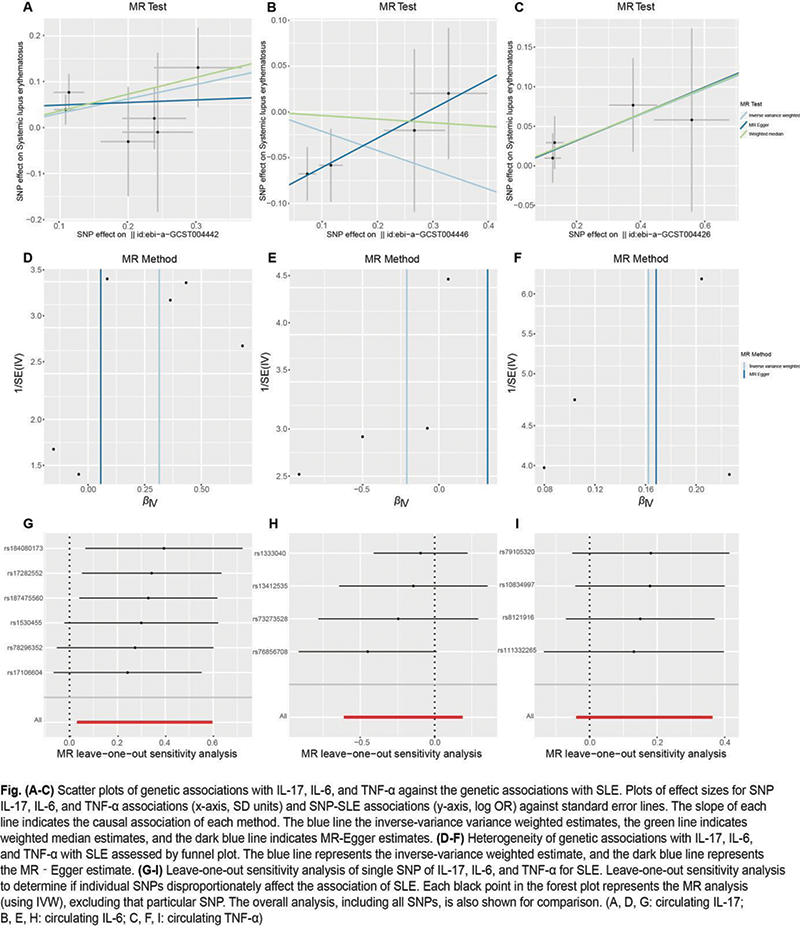
Acknowledgements: NIL.
Disclosure of Interests None Declared.
Keywords: Cytokines and chemokines, Genetics/epigenetics, Systemic lupus erythematosus
DOI: 10.1136/annrheumdis-2023-eular.1048