

Background: There is still a debate whether Behçet syndrome (BS) belongs to the spondyloarthritis (SpA) spectrum. Despite the distinct manifestations of BS and spondyloarthritides, there are shared features such as eye involvement, enthesitis, inflammatory bowel disease, and arthritis across these both inflammatory diseases. Furthermore, both diseases show a strong MHC class I association and genome-wide association studies implicate shared pathogenic pathways between SpA and BS [1].
Objectives: In this study, we aimed to determine the frequency of axial SpA (axSpA) among our BS patients using the Assessment of Spondyloarthritis International Society (ASAS) criteria.
Methods: We included 196 consecutive BS patients under the age of 45 who fulfilled the criteria set by the International Society Group for BS. The patients who meet the ASAS definition of chronic back pain underwent screening for ASAS classification criteria for axSpA. All patients who reported current or past chronic back pain underwent further evaluations including HLA-B27 and C-reactive protein testing, X-ray, and magnetic resonance imaging (MRI) of the sacroiliac joints, in addition to the assessments of other SpA features. Inflammatory back pain (IBP) was assessed by ASAS criteria. The radiographic images were reviewed by two experienced radiologists. A one-sample exact test was used to compare the prevalence of axSpA in BS patients against the general population, which has a axSpA prevalence of 1.4%.
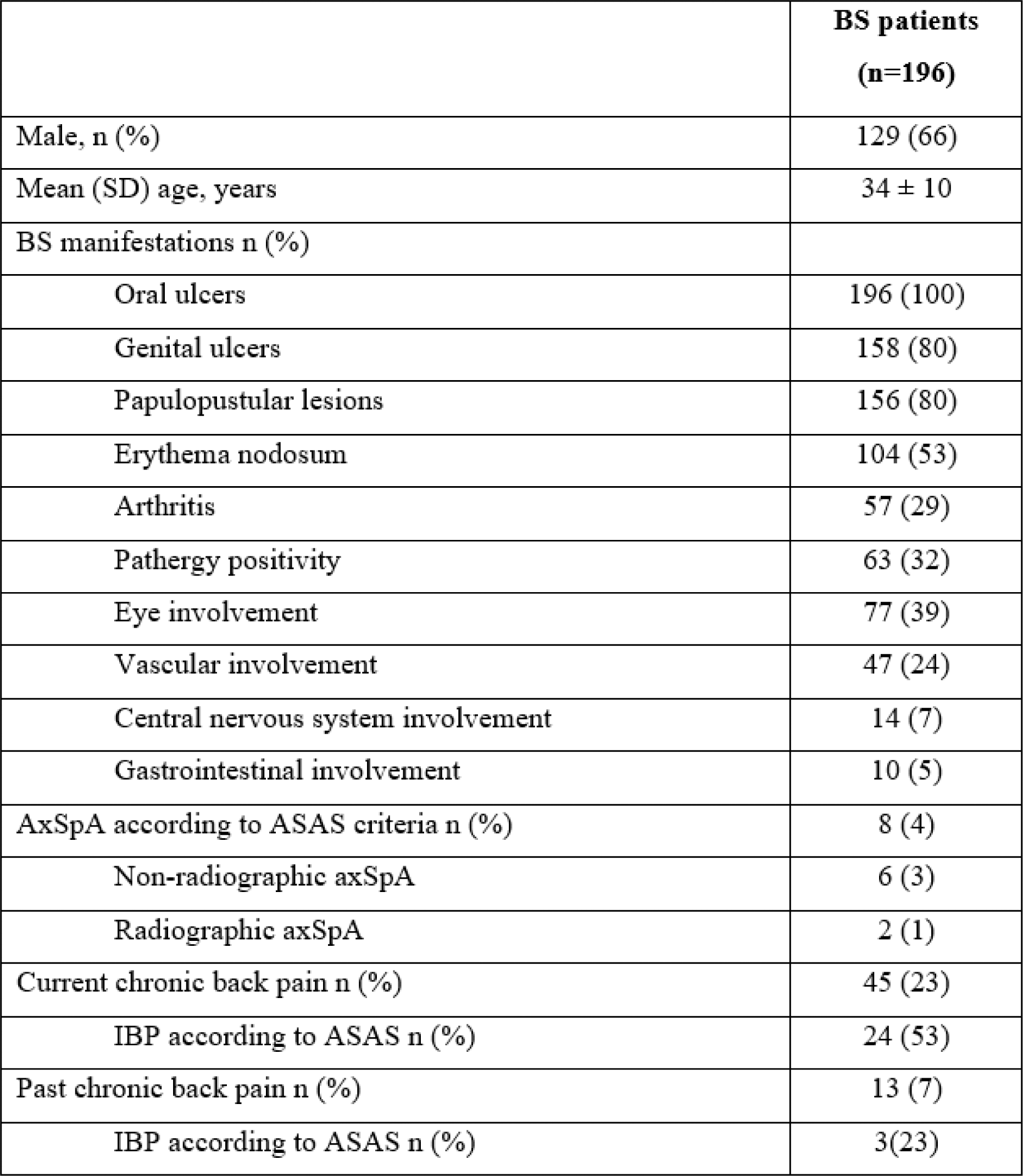
Results: Among 196 BS patients, 45 (23%) had current chronic back pain, and 24 (53%) whom reported as inflammatory. Eight patients (4%; 95% CI 1.8-8; p=0.04) fulfilled axSpA criteria according to ASAS. Two patient was classified as radiographic axSpA and the remaining 6 were classified as non-radiographic axSpA (Table 1). Among the 6 patients with non-radiographic axSpA, one patient fulfilled the imaging arm (MRI positive) while the other 5 patients fulfilled the clinical arm (HLA-B27 positive). Demographics and features of SpA and BS in these 8 patients are presented in the Figure 1. HLA-B27 was positive in 8 (4%) of the total patient population. Out of 13 BS patients with a past history of chronic back pain, only one was classified as radiographic axSpA. This patient manifested with IBP, positive findings of sacroiliitis on X-ray and MRI, arthritis, a good response to NSAID, and a positive family history.
.
Conclusion: The prevalence of axial SpA according to ASAS criteria for axial SpA among BS patients was 4% (95% CI 1.8-8). This is higher compared to that in the general population. Considering that many SpA features are frequently observed in BS patients, it is important to note that in real-life scenarios, BS can mimic SpA, and vice versa. However, certain mucocutaneous and major organ manifestations, like the posterior uveitis. vascular and neurologic involvement, of BS differentiate the two diseases from each other. The mere 80% sensitivity and specificity of the ASAS criteria for axial SpA [2] coupled with a disease concordance bias in a study among hospital cohort further also should be taken in interpreting what we observed.
REFERENCES: [1] McGonagle D, et al. Nat Rev Rheumatol. 2015;11:731-40.
[2] Rudwaleit M et al. Ann Rheum Dis 2009;68:777–83.
Table 1. Demographics and clinical characteristics of the patients
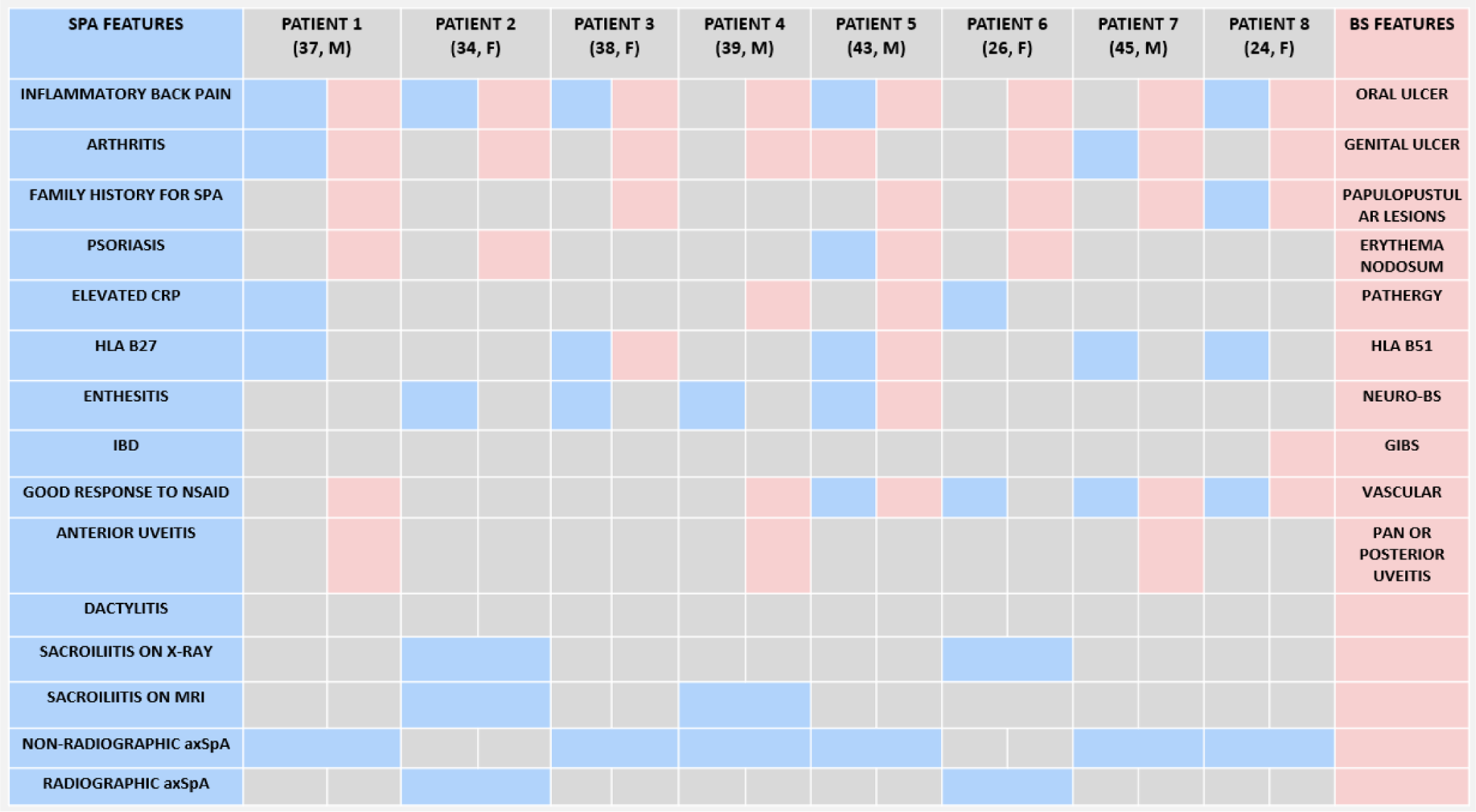
BS and SpA features of 8 BS patients who fulfilled axSpA
Acknowledgements: NIL.
Disclosure of Interests: Melike Melikoglu: None declared, Alihan Ozay: None declared, Sinem Nihal Esatoglu S.N.E has received honorariums for presentations from UCB Pharma, Roche, Pfizer and Merck Sharp Dohme., İbrahim Adaletli: None declared, Fatih Kantarci: None declared, Ahmet Oz: None declared, Erkan Yilmaz: None declared, Gulen Hatemi G.H has received lecture fees from Celgene, Novartis, Abbvie, Amgen, and UCB Pharma, G.H has received consulting fees from Celgene, UCB Pharma, Bayer, and Johnson & Johnson., G.H has received research grant from Celgene., Emire Seyahi: None declared, Serdal Ugurlu: None declared, Didar Ucar: None declared.