

Background: Rheumatoid arthritis (RA) is associated with a heightened 1.5-3-fold risk of developing lymphoma, attributed to elevated systemic inflammation and sustained immune system stimulation. Markers of disease severity and activity in RA strongly correlate with this heightened risk. Recent advancements in therapeutic armamentarium have resulted in improved control of disease activity, potentially influencing lymphoma occurrence in these individuals.
Objectives: To assess the trends in the prevalence of Hodgkin’s and non-Hodgkin’s lymphomas, as well as hospital outcomes in hospitalized patients with underlying RA using the extensive National Inpatient Sample (NIS) database.
Methods: The NIS is the largest publicly available all-payer inpatient healthcare database designed to generate United States regional and national estimates regarding inpatient utilization, access, cost, quality, and outcomes. Unweighted, it contains data from around 7 million hospital stays each year. Weighted, it estimates around 35 million hospitalizations nationally. For our analysis, we utilized data spanning from 2009 to 2019. After appropriately filtering hospitalizations using ICD-9 CM/ICD-10 CM codes, we included hospitalizations of individuals over 18 years old with a primary diagnosis of RA and a secondary diagnosis of lymphoma (Hodgkin’s and non-Hodgkin’s lymphoma). The analysis accounted for NIS clustering, survey design, stratification, and weights. Categorical data were presented as frequencies and percentages, while continuous variables were expressed as means with standard deviations. To assess trends in lymphoma prevalence among RA hospitalizations, we employed the Jonckheere-Terpstra trend test. Additionally, we evaluated various hospital outcomes for the cohort, focusing primarily on in-hospital mortality and secondarily on age, length of hospital stays in days, and cost of care in US dollars. Categorical and continuous variables were analyzed using the Pearson chi-square test and Wilcoxon rank-sum test, respectively. Statistical significance was determined at a p-value of <0.05 for all conducted tests. All analyses were performed using SAS, version 9.4 (SAS Institute Inc.).
Results: Identified over a decade, from 2009 to 2019, a total of 53,439 patients had a primary diagnosis of RA along with secondary diagnoses of Hodgkin’s or non-Hodgkin’s lymphoma. Figure 1 displays the baseline comorbidities of the cohort. Figure 2 illustrates the trends in lymphoma prevalence.
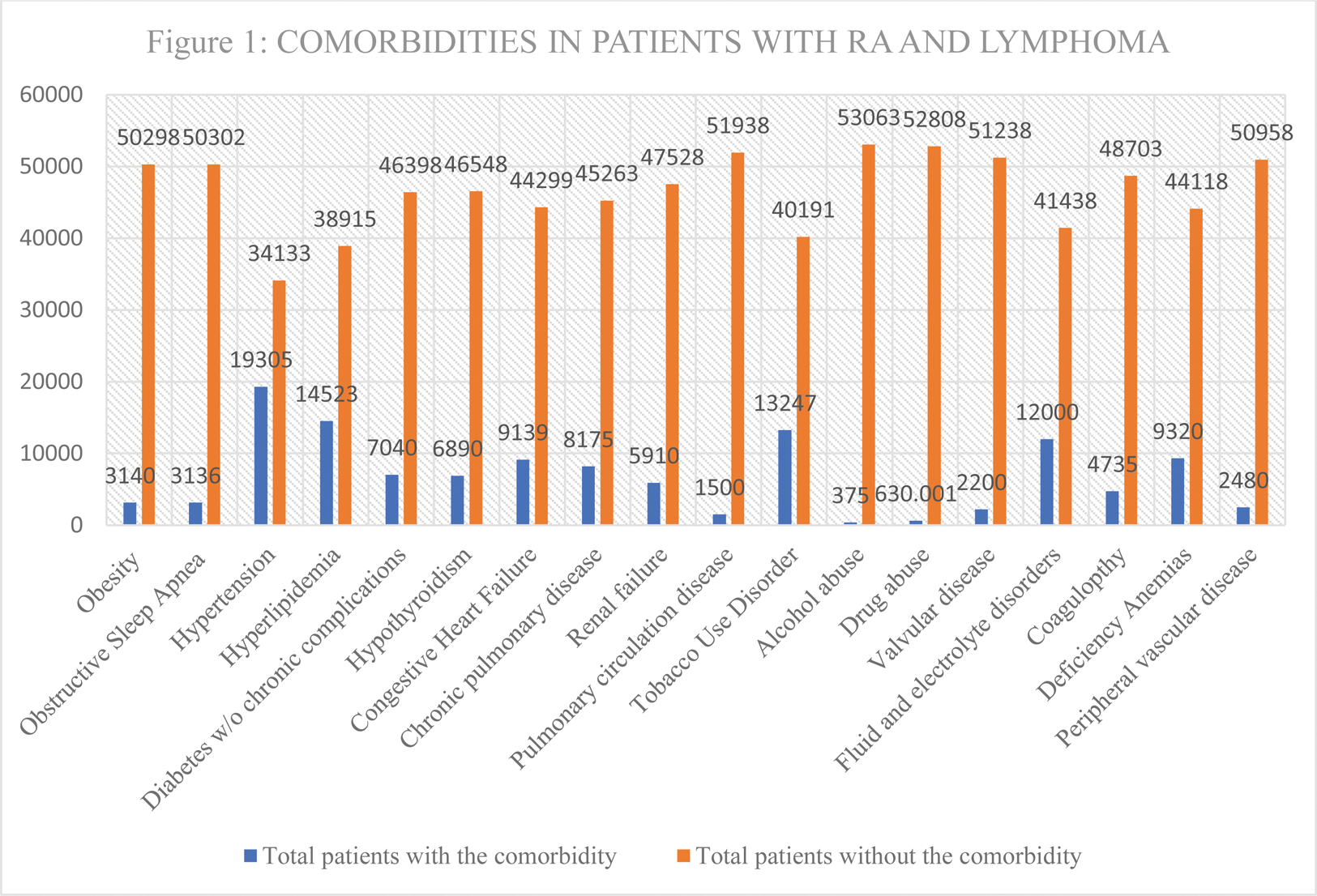
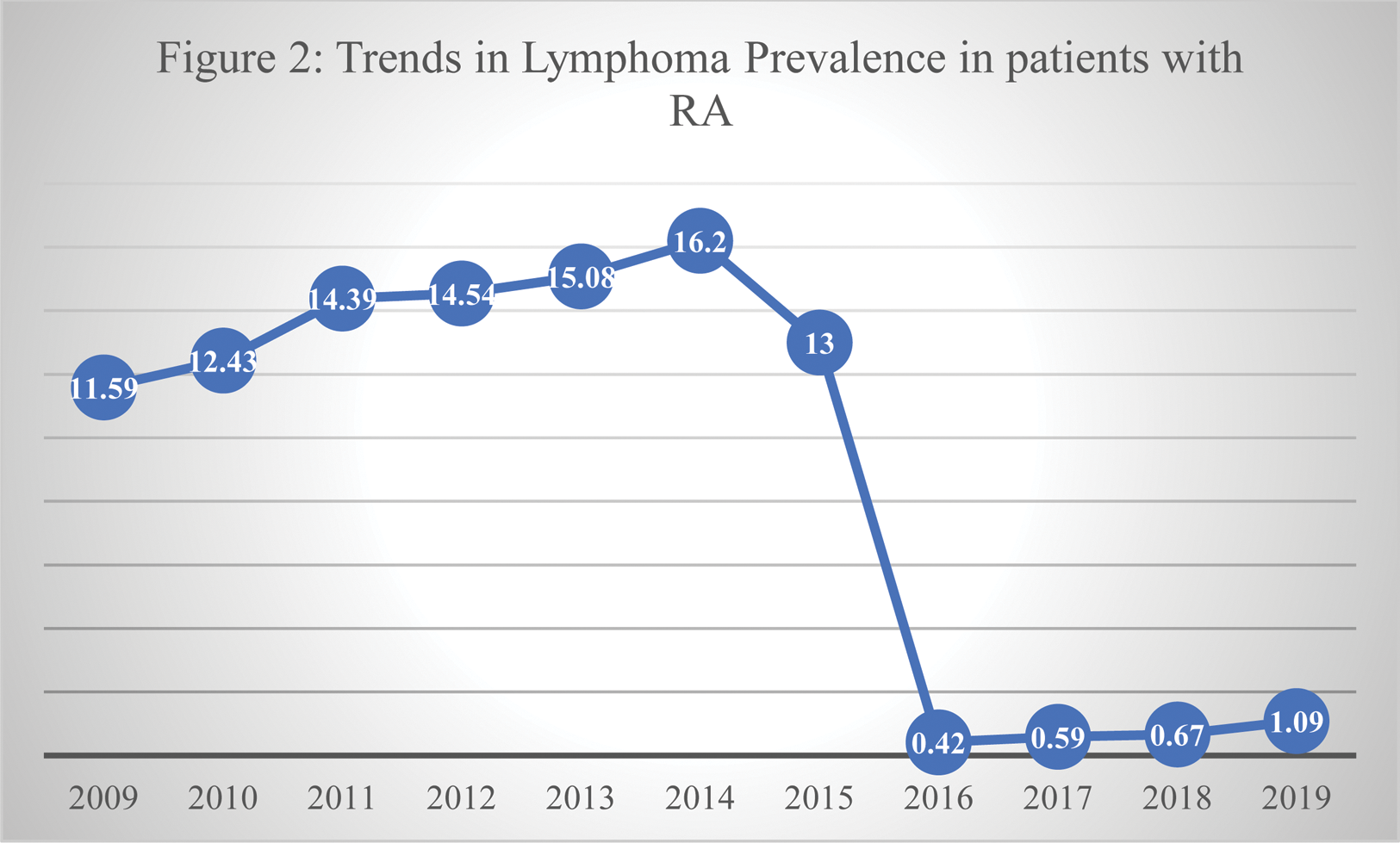
The average in-hospital mortality rate was 4.53% (2419 patients), with an average age of hospitalization being 70.10 years, an average length of stay of 6.27 days, and an average cost of hospital stay amounting to $14741.70.
Conclusion: The prevalence of lymphoma showed a significant decline, dropping sharply from 11.59% in 2009, when the study commenced, to its lowest recorded level of 0.42% in 2016, with the peak prevalence in 2013 reaching 15.08%. This reduction in lymphoma prevalence appears to align with advancements in the therapeutic management of RA, resulting in lower disease activity and subsequently reduced lymphoma risk. Further investigations are necessary to pinpoint the specific reasons for this decline. Understanding these factors could improve patient care and alleviate the considerable economic burden, as evidenced by the approximate $17,000 cost incurred during a week-long hospital stay for these patients.
REFERENCES: [1] Kedra J, Seror R, Dieudé P, Constantin A, Toussirot E, Kfoury E, Masson C, Cornec D, Dubost JJ, Marguerie L, Ottaviani S, Grados F, Belkhir R, Fain O, Goupille P, Sordet C, Fautrel B, Philippe P, Piperno M, Combe B, Lambotte O, Richez C, Sellam J, Sené T, Denis G, Lequerre T, Lazure T, Mariette X, Nocturne G. Lymphoma complicating rheumatoid arthritis: results from a French case-control study. RMD Open. 2021 Sep;7(3):e001698. doi: 10.1136/rmdopen-2021-001698. PMID: 34470830; PMCID: PMC8413949.
[2] D. P. M. Symmons, Lymphoma and rheumatoid arthritis—again, Rheumatology, Volume 46, Issue 1, January 2007, Pages 1–2,
Acknowledgements: NIL.
Disclosure of Interests: None declared.