

Background: Lupus, a rare chronic autoimmune disorder negatively impacting patients’ quality of life, productivity, survival, exacts a high burden on the healthcare system. Patients with lupus are frequently affected by neuropsychiatric manifestations (up to 40% with depression and up to 80% with cognitive dysfunction[1]). These are often incapacitating, sometimes with life-threatening consequences. Neuropsychiatric manifestations might develop before a diagnosis for lupus is established and could occur independently of lupus disease activity. Among mental and behavioral disorders (MDD), depression is reported to adversely affect medication adherence, resource use and outcomes[2]. While few international studies have reported on the disease and economic burden associated with neuropsychiatric lupus, little data exist on the prevalence of MDD, and associated healthcare resource use and costs in France.
Objectives: This study evaluates the inpatient and day hospital prevalence, healthcare resource use and costs associated with neuropsychiatric manifestations of lupus between 2018 and 2022 in France.
Methods: Retrospective analyses were conducted using the French national hospital claims database (PMSI, Medical surgical and obstetrics (MSO)[3]). Patients hospitalized for Systemic Lupus Erythematosus (SLE; ICD10 M32.X) and/or Lupus Erythematosus (LE; ICD10 L93.X) recorded as main, secondary and/or associated diagnosis and MDD (fatigue, major depressive disorder, or other mood disorders) recorded as main and/or secondary diagnosis between January 2018 and December 2021 were included and followed-up until their date of death or end of study (December 2022). The occurrence of all-cause hospitalizations, hospitalizations for lupus, MDD, dialysis and renal disorders over the follow-up period was described and their hospital costs estimated.
Results: Out of 27,243 patients with lupus identified in a hospital setting between 2018 and 2021, 799 (3%) lupus patients presented a diagnosis of MDD in the hospital setting, with 43% with SLE, 24% with LE and 33% with both SLE and LE.
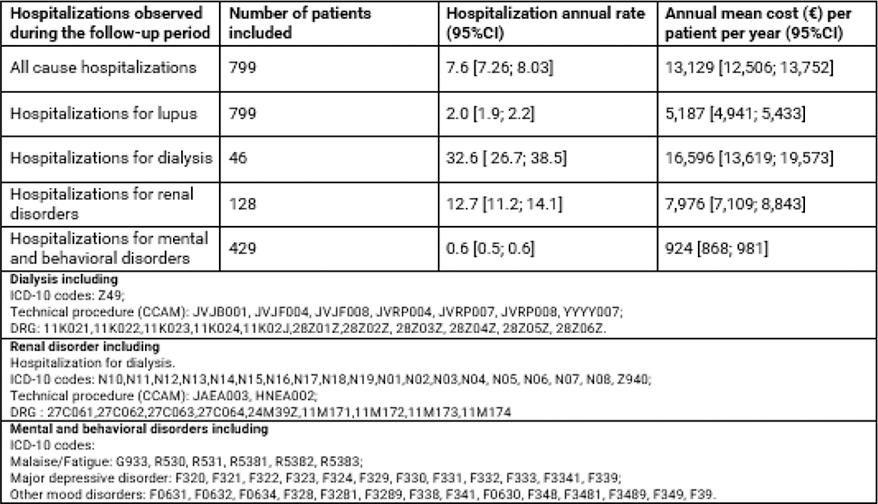
Most of the patients were adults (97%), females (85%), with a mean age of 54 (±18.9) years at time of first hospitalization for lupus. Sixty-eight percent of patients had malaise and fatigue, 30% major depressive disorders, and 5% other mood disorders. In 61% of patients, the first hospitalization with MDD was observed on average one year before the first hospitalization for lupus (1.2 (±1.3) years). Patients also presented with several non-psychiatric comorbidities and/or complications of lupus, such as cardiovascular diseases (33% of patients) and kidney disorders (21%). Sixty-eight percent of patients lived in an urban area and 13% in areas considered to be the most deprived (high proportion of unemployment, low income, low proportion of people with higher degree, etc.). The annual hospitalization rates and hospital costs per patient per year during the follow-up period are described in Table 1. The annual mean cost per patient for all-cause hospitalizations was €13,129, of which 40% was due to hospitalizations for lupus. On average, patients were hospitalized with lupus twice per year. Fifty percent of the patients had at least one hospitalization for MDD over the follow-up period.
Conclusion: This nationwide study brings new evidence on the impact of lupus and the neuropsychiatric manifestations of lupus on the French health care system. Overall, more than half of patients were hospitalized with a diagnosis of MDD during the follow-up. Yet, these numbers may be underestimated considering that most MDD are treated outside the hospital and/or in psychiatric centers in France (data not reported in PMSI MSO). Additional research is needed to further characterize the impact of MDD management, healthcare resource use and associated costs in patients with lupus and psychiatric manifestations in France, using the specific dataset for psychiatric care available within PMSI.
REFERENCES: [1] Meszaros ZS et al., J Clin Psychiatry. 2012
[2] Julian LJ et al., Arthritis Rheum. 2009
[3] ATIH, Methodological guide PMSI MSO 2023
Table 1. Annual hospitalization rates by type of hospitalizations
Acknowledgements: NIL.
Disclosure of Interests: Nicoleta Petrica Consulting activity within Alira Health for several Pharmaceutical clients., Nathan Cohen Consulting activity within Alira Health for several Pharmaceutical clients., Maria Pini Consulting activity within Alira Health for several Pharmaceutical clients., Mathieu Rosé Former Pharma employee, Consulting activity within Alira Health for several Pharmaceutical clients., Jean-Francois Ricci Former Pharma employee, Consulting activity within Alira Health for several Pharmaceutical clients.