

Background: Systemic vasculitides are a group of inflammatory multisystem diseases with recurrent relapses and chronic damage due to disease and its treatments. The extent to which having this condition impacts the psychological health of patients is yet to be fully understood.
Objectives: To quantify the psychological impact of living with systemic vasculitides.
Methods: We cross-sectionally evaluated a cohort of patients with systemic vasculitides seen at diagnosis or follow-up in our center, between April 1 st and December 31 st , 2023. Data collected from each patient included their demographic and clinical data, as well as their medical history.
We administered the symptom checklist revised (SCL-90-R) to measure distress related to 9 psychological dimensions, i.e. somatization (SOM), obsessive compulsion (OC), interpersonal sensitivity (IS), depression (DEP), anxiety (ANX), hostility (HOS), phobic anxiety (PHOB), paranoid ideation (PAR), psychoticism (PSY), and providing 3 global indices of distress, i.e. global severity index (GSI, the average symptom intensity), positive symptom distress index (PSDI, average level of distress for those items that were endorsed), and positive symptom total (PST, i.e. total symptoms endorsed). Distress was categorized in 4 intensity levels (null, low, moderate and high) with respect to the Italian reference population. We applied loglinear model to investigate if different vasculitis vessel types correlated with different psychological distress.
Results: By using the SCL-90-R checklist, we screened a total of 171 patients affected by systemic vasculitides (females 48.5%, mean age 65 years old, range: 21-88): 64% had small vessel vasculitis (SVV, of which 89% were ANCA-associated vasculitides), 29% had large vessel vasculitis (LVV, of which 79% were giant cell arteritis), 7% had variable vessel vasculitis (VVV, Behcet’s disease).
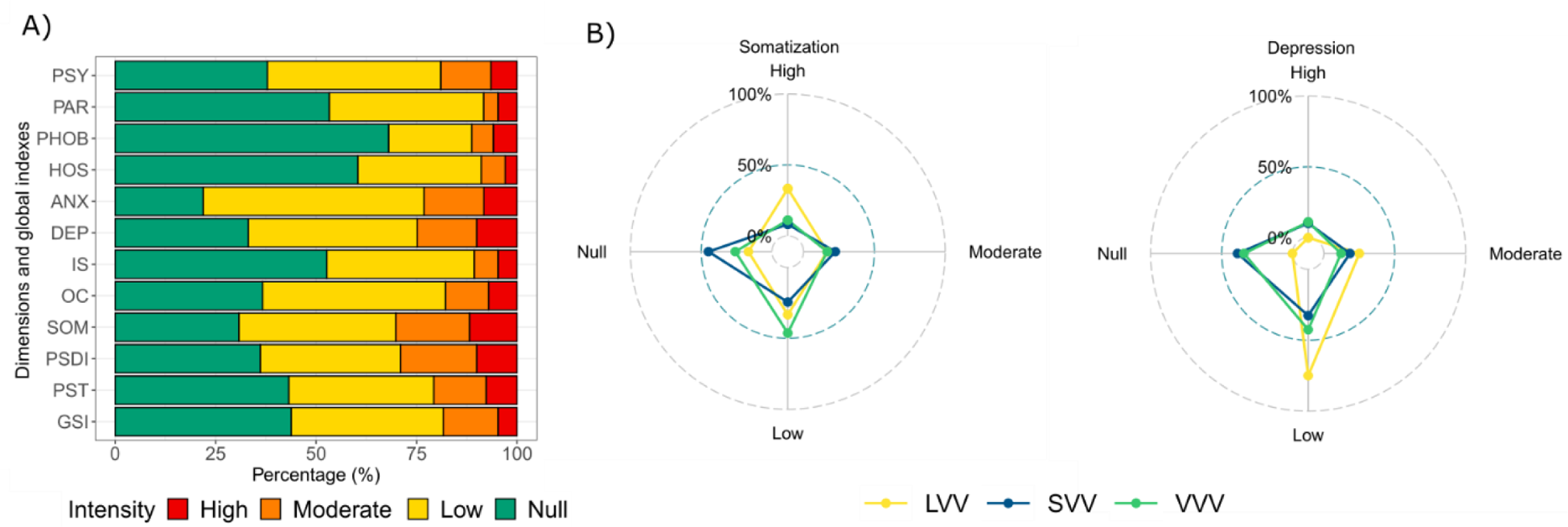
Eight % of patients reported moderate-to-high intensity for PAR and HOS, while more than 20% for DEP and ANX. Thirty % of patients reported moderate-to-high intensity for SOM, which may be expected considering the confounding effect of being affected by systemic vasculitides. Less than 5% reported no symptoms in any dimensions, while 45% reported at least one dimension with moderate-to-high intensity, and 13% more than 4 dimensions (as shown in Figure 1A, representing percentage of outpatient with psychological distress and its intensity for each of the 9 dimensions and 3 global indexes).
Active disease (as assessed by Birmingham vasculitis activity score >0) was associated with DEP, ANX, PSY, and PST (p<0.05); prednisone ≥5 mg/day was associated with ANX (p<0.05), while no dimensions were associated with different categories of immunosuppressive therapies. Notably, severe damage (Vasculitis Damage Index ≥5) associated with SOM, OC, DEP, ANX, GSI, and PSDI (p<0.05).
Loglinear models showed associations of different vasculitis vessel types only with DEP (p=0.01) and SOM (p=0.03), as shown in the radar plots (Figure 1B).
Conclusion: Patients affected by systemic vasculitides showed psychological distress in various symptomatic dimensions with respect to the Italian reference population, showing significant association with disease activity, glucocorticoid use, vasculitis vessel types, and particularly with severe damage. Our findings showed the need for psychological screening to identify distress due to vasculitis, aiming to reduce it with psychological interventions.
REFERENCES: [1] Derogatis, L.R. and Unger, R. Symptom Checklist-90-Revised (2010).
Acknowledgements: NIL.
Disclosure of Interests: None declared.