

Background: Pauci-immune glomerulonephritis (GN) is a renal manifestation of anti-neutrophil cytoplasmic antibody (ANCA)-associated vasculitis (AAV), occurring in 70-100% of cases. Kidney involvement in AAV can lead to chronic kidney disease (CKD), which progresses to end-stage renal disease (ESRD) in approximately 20% of cases. When patients show positive ANCA results accompanied by urinary abnormalities such as hematuria and proteinuria, pauci-immune GN is suspected. However, there have been some cases in which patients with positive ANCA results revealed unexpected pathologies during tissue examination.
Objectives: We aimed to investigate and compare the characteristics of patients showing positive ANCA results with pauci-immune GN to those without, determined based on renal tissue examination.
Methods: We retrospectively reviewed the electronic medical records of patients who underwent renal biopsy showing positive ANCA results from October 2013 to August 2021 at a single tertiary center in Seoul, South Korea. Logistic regression analysis was performed to identify the variables associated with pauci-immune GN among the patients who underwent renal biopsy and showed positive ANCA results.
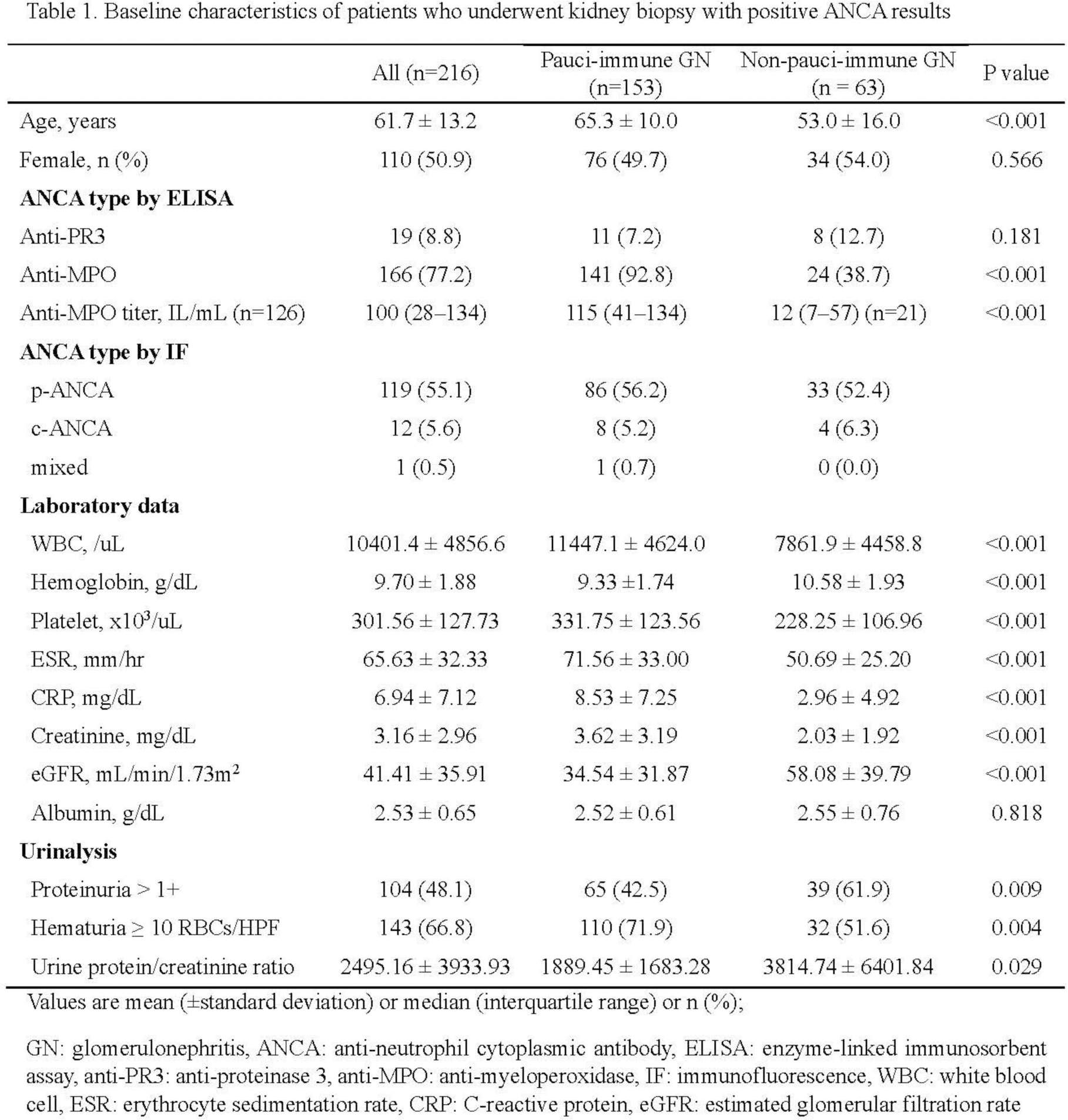
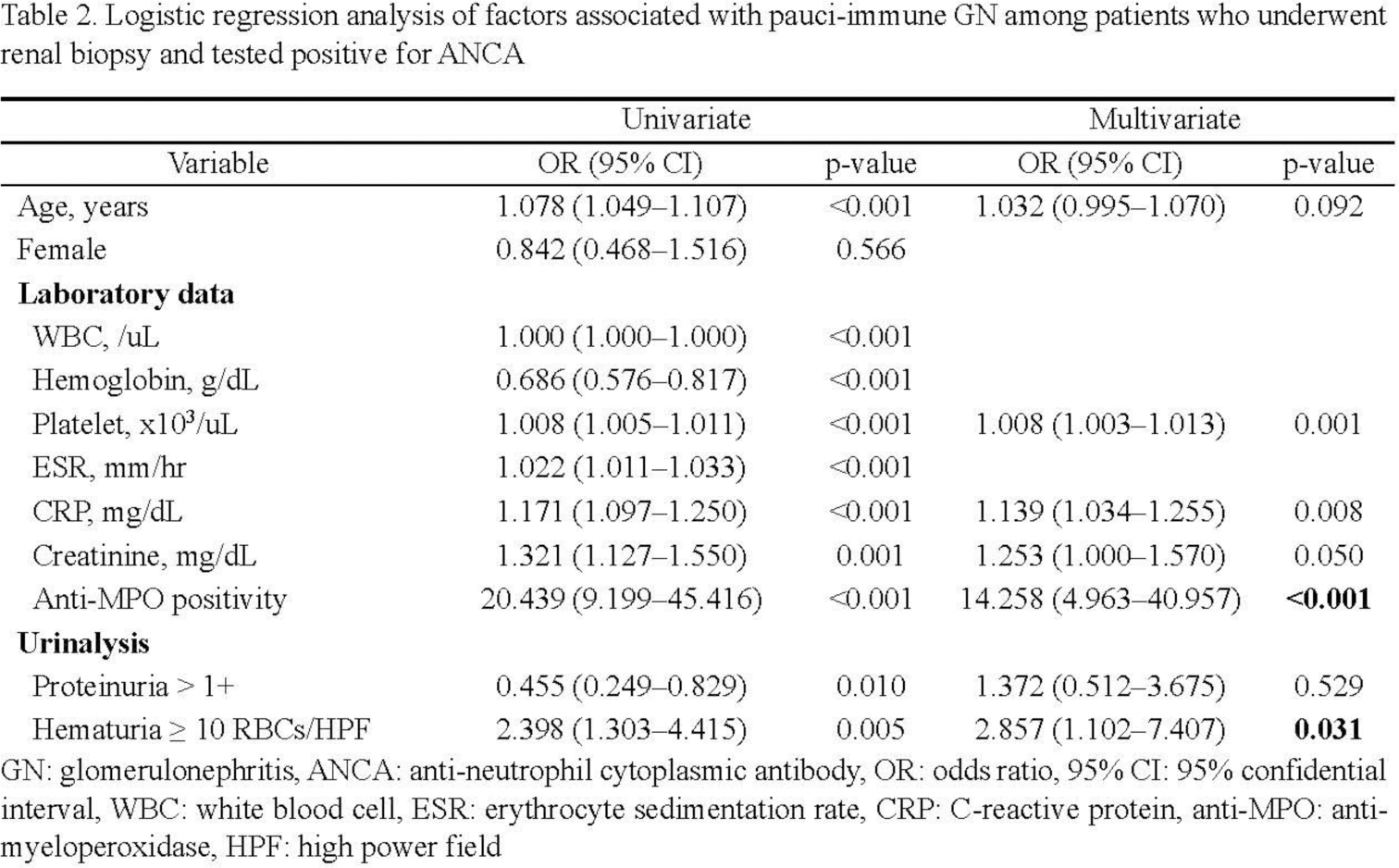
Results: A total of 216 patients who underwent renal biopsy showing positive ANCA results were included in our analysis. The mean age of the patients was 61.7 ± 13.2 years, with 50.9% of them being female. Among all patients, 153 (70.8%) were diagnosed with pauci-immune GN through renal biopsy, while 63 (29.2%) were diagnosed with other kidney diseases. There was no statistically significant difference in terms of gender between the pauci-immune GN group and the non-pauci-immune GN group. However, the pauci-immune GN group’s mean age (65.3 years) was higher than that of the non-pauci-immune GN group (53.0 years). Autoantibody analysis revealed that 92.8% of the pauci-immune GN group tested positive for anti-myeloperoxidase(MPO), whereas only 38.7% in the non-pauci-immune GN group showed positivity (p < 0.001). Furthermore, the pauci-immune GN group showed a median anti-MPO titer of 115 IU/mL, which was significantly higher than the non-pauci-immune GN group’s median titer of 12 IU/mL (p < 0.001). Regarding blood chemistry, the pauci-immune GN group showed a higher white blood cell (WBC) count, lower hemoglobin levels, higher platelet count, elevated erythrocyte sedimentation rate (ESR), increased C-reactive protein (CRP), and higher creatinine levels compared to the non-pauci-immune GN group, all of which were statistically significant differences. Urinalysis was determined according to the Birmingham Vasculitis Activity Score (BVAS) criteria, which indicated that the pauci-immune GN group had fewer patients with proteinuria greater than 1+ and more patients with hematuria greater than 10 per high power field compared to the non-pauci-immune GN group. The renal tissue analysis of the non-pauci-immune GN group revealed diverse pathological findings. The most prevalent conditions included IgA nephritis at 20.6%, followed by lupus nephritis at 17.5% of the group. Additional identified pathologies included membranous glomerulonephritis, diabetic nephropathy, chronic nephropathy, and several others. Considering the correlations among blood chemistry levels, a multivariate analysis was conducted to adjust for age, platelet count, CRP, creatinine, and proteinuria levels. The results of the analysis revealed a significant association between anti-MPO positivity (OR: 14.258; 4.963–40.957) and hematuria (OR: 2.857; 1.102–7.407) with the presence of pauci-immune GN observed in renal tissue examination.
Conclusion: In the analyzed cohort of patients, approximately 70% of those who underwent renal biopsy and showed positive ANCA results were diagnosed with pauci-immune GN. There was a significant association between anti-MPO positivity and hematuria on microscopy with pauci-immune GN. Our findings emphasize the importance of identifying high-risk antibody profiles and urinalysis associated with pauci-immune GN.
REFERENCES: NIL.
Acknowledgements: NIL.
Disclosure of Interests: None declared.