

Background: Inflammatory myopathy (IM) occurs in systemic sclerosis (SSc) in around 14-25% of patients, generally associated with worse prognosis. Muscular histopathological characteristics have shown to be heterogeneous, although some studies have found fibrosis to be a common lesion in SSc muscle biopsies, being associated with a more severe disease with diffuse cutaneous involvement and higher mortality.
Objectives: To describe the clinical and histological features of IM associated with SSc and to analyze whether there are differences compared to other IIM subgroups.
Methods: All patients with a clinical diagnosis of idiopathic inflammatory myopathy (IIM) followed at the Rheumatology Department of the University Hospital 12 Octubre between 1986 and 2023, having at least one muscular biopsy were selected. Among these patients, those who also met the 2017 ACR/EULAR classification criteria for SSc were identified.
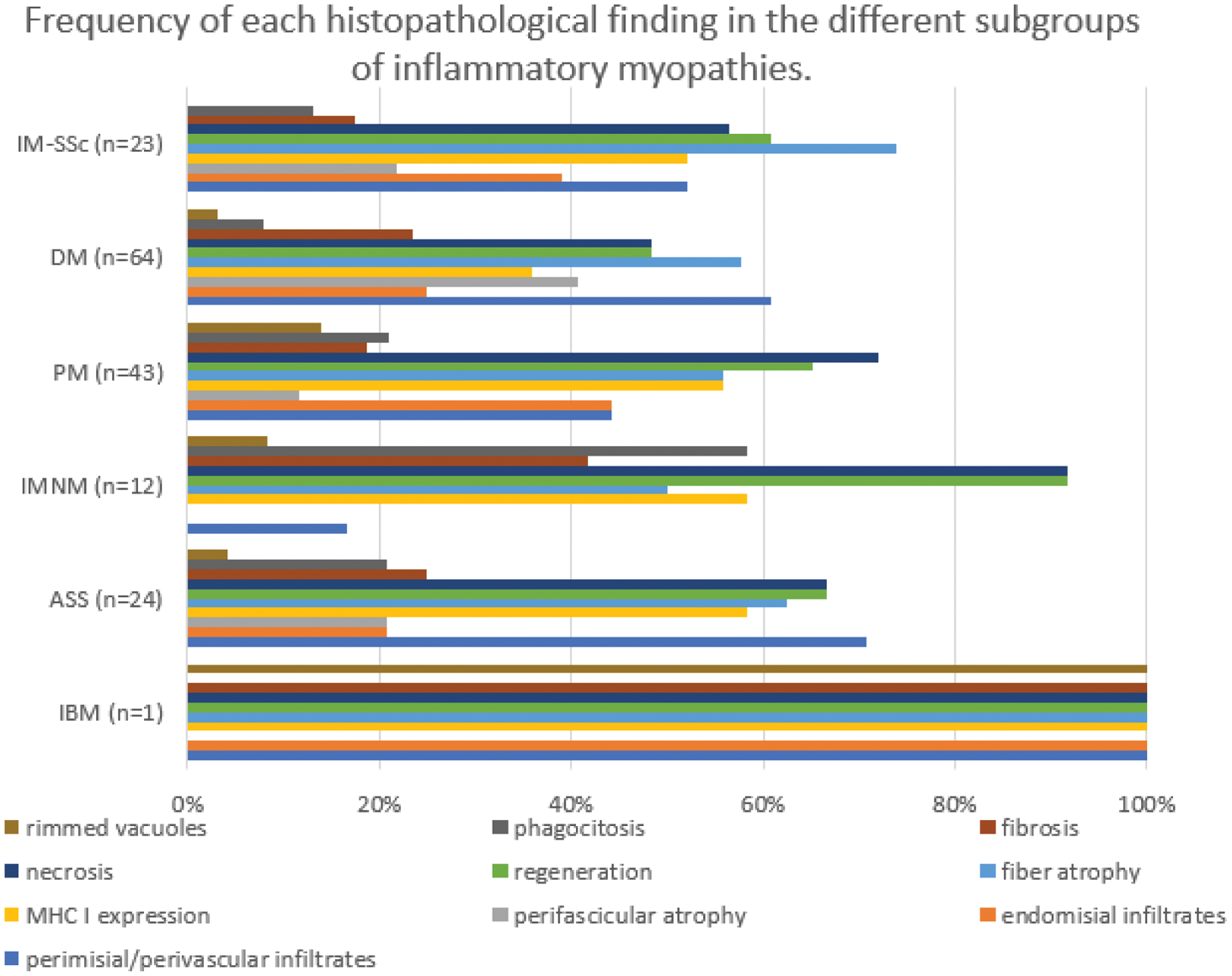
Results: From 276 patients with IIM, 167 had at least one muscular biopsy. Twenty-three (13.8%) met the SSc classification criteria, and were included in the overlap subgroup (IM-SSc). Other IIM clinical subgroups are presented in Figure 1. The most frequent findings in IIM-SSc muscular biopsies were: muscle fiber atrophy (73.9%), regeneration (60.9%), and necrosis (56.5%). The most common histopathological pattern was nonspecific myopathy (52.2%). No patient was diagnosed with necrotizing myopathy (IMNM) based on biopsy. Fibrosis was an infrequent lesion (n = 4, 17.4%) and was associated with lower CK levels at disease onset (445 ± 359, p = 0.01). When comparing IM-SSc patients with other IIM subgroups, there were no significant histopathological differences (Figure 2).
Conclusion: SSc associated IM is a heterogeneous entity with no significant histopathological differences from other subgroups of IIM. Further studies are needed to better characterize this patient’s subgroup.
DM: dermatomyositis, PM: polimyositis; IIM-SSc: idiopathic inflammatory myopathy associated to systemic sclerosis; ASS: antisynthetase syndrome; IMNM: immunomediated necrotizing myopathy; IBM: inclusion body myositis
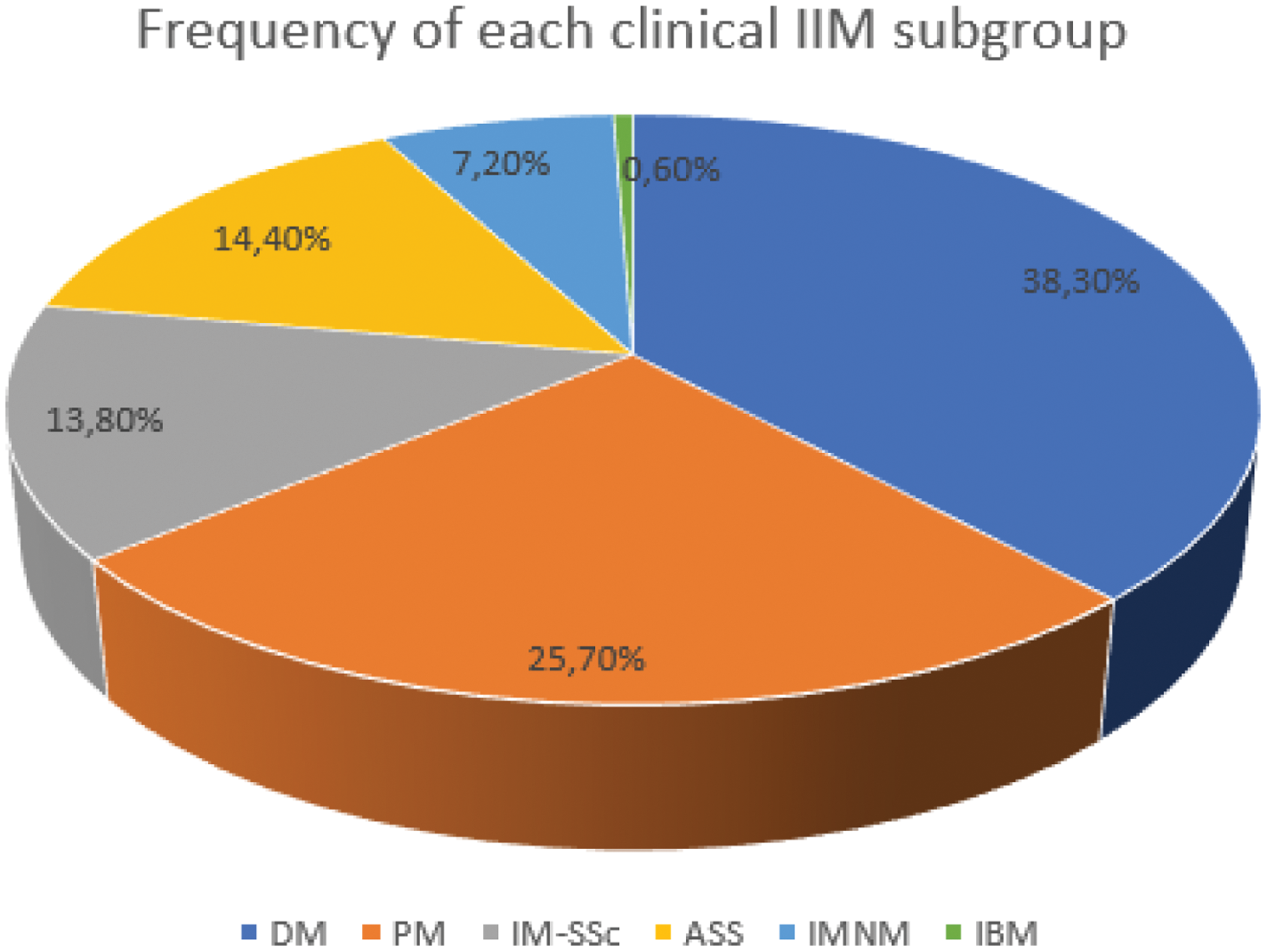
IIM-SSc: idiopathic inflammatory myopathy associated to systemic sclerosis; DM: dermatomyositis; PM: polymyositis; IMNM: immunomediated necrotizing myopathy; ASS: antisynthetase syndrome; IBM: inclusion body myositis; MHC: major histocompatibility complex.
REFERENCES: [1] Selva-O’Callaghan A, Pinal-Fernandez I, Trallero-Araguás E, Milisenda JC, Grau-Junyent JM, Mammen AL. Classification and management of adult inflammatory myopathies. Lancet Neurol. 2018 Sep;17(9):816-828. doi: 10.1016/S1474-4422(18)30254-0.
[2] Paik JJ. Myopathy in scleroderma and in other connective tissue diseases. Curr Opin Rheumatol. 2016 Nov;28(6):631-5. doi: 10.1097/BOR.0000000000000336.
[3] Medsger TA Jr, Rodnan GP, Moossy J, Vester JW. Skeletal muscle involvement in progressive systemic sclerosis (scleroderma). Arthritis Rheum. 1968 Aug;11(4):554-68. doi: 10.1002/art.1780110405.
[4] Paik JJ, Wigley FM, Lloyd TE, Corse AM, Casciola-Rosen L, Shah AA, Boin F, Hummers LK, Mammen AL. Spectrum of Muscle Histopathologic Findings in Forty-Two Scleroderma Patients With Weakness. Arthritis Care Res (Hoboken). 2015 Oct;67(10):1416-25. doi: 10.1002/acr.22620.
[5] Lefebvre F, Giannini M, Ellezam B, Leclair V, Troyanov Y, Hoa S, Bourré-Tessier J, Satoh M, Fritzler MJ, Senécal JL, Hudson M, Meyer A, Landon-Cardinal O. Histopathological features of systemic sclerosis-associated myopathy: A scoping review. Autoimmun Rev. 2021 Jul;20(7):102851. doi: 10.1016/j.autrev.2021.102851.
[6] Matas-García A, Guillén-Del-Castillo A, Kisluk B, Selva-O’Callaghan A, Espinosa G, Prieto-González S, Moreno Lozano P, Garrabou G, Grau-Junyent JM, Simeon-Aznar CP, Milisenda JC. Clinico-pathological phenotypes of systemic sclerosis-associated myopathy: analysis of a large multicentre cohort. Rheumatology (Oxford). 2023 Feb 6;62(SI):SI82-SI90. doi: 10.1093/rheumatology/keac361.
Acknowledgements: NIL.
Disclosure of Interests: None declared.
© The Authors 2025. This abstract is an open access article published in Annals of Rheumatic Diseases under the CC BY-NC-ND license (