

Background: Cross-hormone therapy (CHT) is the cornerstone of gender-affirming treatment for transwomen. While CHT has been extensively studied for its effects on cardiovascular health, its impact on bone health, particularly bone mineral density (BMD), requires further investigation. This updated meta-analysis evaluates the effect of CHT on changes in BMD in transwomen over a 12-month period, focusing on the femoral neck, lumbar spine, and total femur.
Objectives: The primary objective of this meta-analysis was to assess changes in BMD at the femoral neck, lumbar spine, and total femur in trans women undergoing CHT over a 12-month period. The analysis aimed to determine whether CHT positively or negatively affects bone density.
Methods: A systematic search was conducted to identify studies measuring BMD in trans women before and after 12 months of CHT. Data were extracted from studies reporting mean BMD values at the femoral neck, lumbar spine, and total femur, along with corresponding standard deviations. Random-effects models were used to calculate the mean differences (MD) in BMD between baseline and 12 months after CHT. Heterogeneity between studies was assessed using the I² statistic, and the overall effect was tested using z-scores.
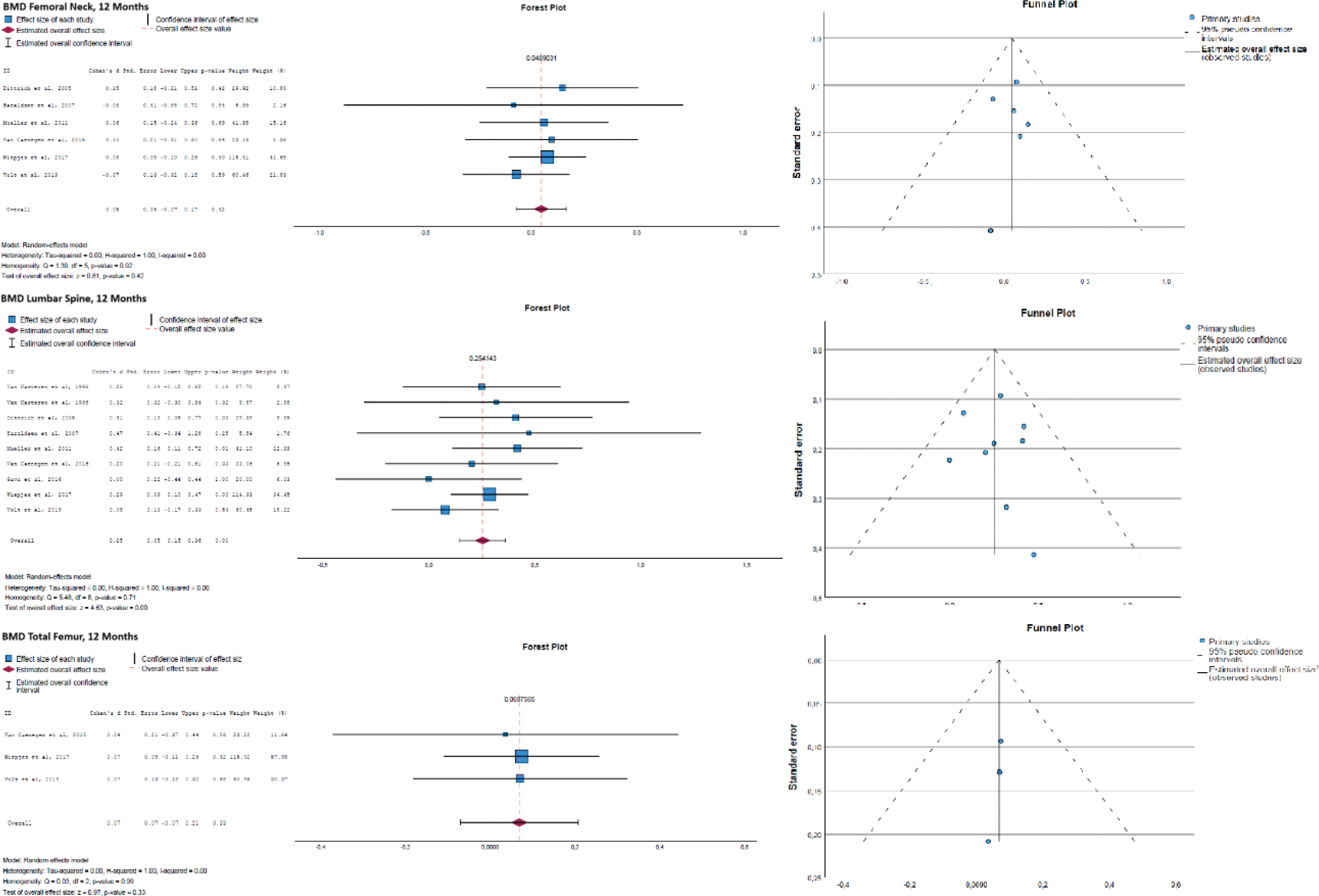
Results: The analysis included 9 studies reporting BMD outcomes in trans women. At the femoral neck, the mean difference in BMD was 0.004 g/cm² (95% CI [−0.03, 0.04]), indicating no significant change. A significant increase in BMD was observed at the lumbar spine, with a mean difference of 0.03 g/cm² (95% CI [0.01, 0.05]). At the total femur, a modest increase was also found, with a mean difference of 0.008 g/cm² (95% CI [−0.01, 0.03]). Heterogeneity across studies was low for all regions, supporting the robustness of the findings. Funnel plots revealed no significant evidence of publication bias.
Conclusion: Cross-hormone therapy in trans women is associated with modest but significant improvements in bone mineral density at the lumbar spine over 12 months, while maintaining stable BMD at the femoral neck and total femur. These findings underscore the safety of CHT in preserving and potentially enhancing bone health in trans women during the first year of treatment.
REFERENCES: [1] van Kesteren P, Lips P, Gooren LJ, Asscheman H, Megens J. Long-term follow-up of bone mineral density and bone metabolism in transsexuals treated with cross-sex hormones. Clin Endocrinol (Oxf). 1998; 48:347–54.
[2] Dittrich R, Binder H, Cupisti S, Hoffmann I, Beckmann MW, Mueller A. Endocrine treatment of male-to-female transsexuals using gonadotropin-releasing hormone agonist. Exp Clin Endocrinol Diabetes. 2005; 113:586–9.
[3] Haraldsen IR, Haug E, Falch J, et al. Cross-sex pattern of bone mineral density in early onset gender identity disorder. Horm Behav 2007; 52:334–343.
[4] Mueller A, Zollver H, Kronawitter D, et al. Body composition and bone mineral density in maleto-female transsexuals during cross-sex hormone therapy using gonadotrophin-releasing hormone agonist. Exp Clin Endocrinol Diabetes. 2011; 119:95–100.
[5] Van Caenegem E, Wierckx K, Taes Y, et al. Preservation of volumetric bone density and geometry in trans women during cross-sex hormonal therapy: a prospective observational study. Osteoporos Int. 2015; 26:35–47.
[6] Gava G, Cerpolini S, Martelli V, Battista G, Seracchioli R, Meriggiola MC. Cyproterone acetate versus leuprolide acetate in combination with transdermal oestradiol in transwomen: a comparison of safety and effectiveness. Clin Endocrinol (Oxf). 2016; 85:239–46.
[7] Wiepjes CM, Vlot MC, Klaver M, Nota NM, de Blok CJ, de Jongh RT, Lips P, Heijboer AC, Fisher AD, Schreiner T, T’Sjoen G, den Heijer M. Bone Mineral Density Increases in Trans Persons After 1 Year of Hormonal Treatment: A Multicenter Prospective Observational Study. J Bone Miner Res 2017 6;32(6):1252–1260.
[8] Vlot MC, Wiepjes CM, de Jongh RT, T’Sjoen G, Heijboer AC, den Heijer M. Gender-Affirming Hormone Treatment Decreases Bone Turnover in Transwomen and Older Transmen. J Bone Miner Res. 2019 Oct;34(10):1862-1872. doi: 10.1002/jbmr.3762. Epub 2019 Aug 19. PMID: 31099910; PMCID: PMC6852079.
Acknowledgements: NIL.
Disclosure of Interests: None declared.
© The Authors 2025. This abstract is an open access article published in Annals of Rheumatic Diseases under the CC BY-NC-ND license (