

Background: Systemic sclerosis (SSc) is a rare, chronic connective tissue disease characterized by fibrosis of the skin and internal organs, vasculopathy, and autoimmunity. SSc is typically categorized into three subtypes based on the extent of skin involvement: diffuse cutaneous SSc (dcSSc), limited cutaneous SSc (lcSSc), and sine scleroderma. Additionally, SSc can coexist with other rheumatic diseases, such as rheumatoid arthritis (RA), Sjögren’s disease (SjD), and systemic lupus erythematosus (SLE), collectively referred to as “overlap syndromes” (OS).
Objectives: This study aimed to compare the clinical characteristics of limited and diffuse SSc patients with and without overlap syndromes.
Methods: The Turkish Systemic Sclerosis Registry prospectively enrolls patients with SSc or very early diagnosis of systemic sclerosis (VEDOSS) with a disease duration of ≤3 years. Of the 306 patients registered, 251 who fulfilled the 2013 ACR/EULAR classification criteria were included in this analysis. Demographic, clinical, and laboratory characteristics of lcSSc and dcSSc patients with and without OS were compared.
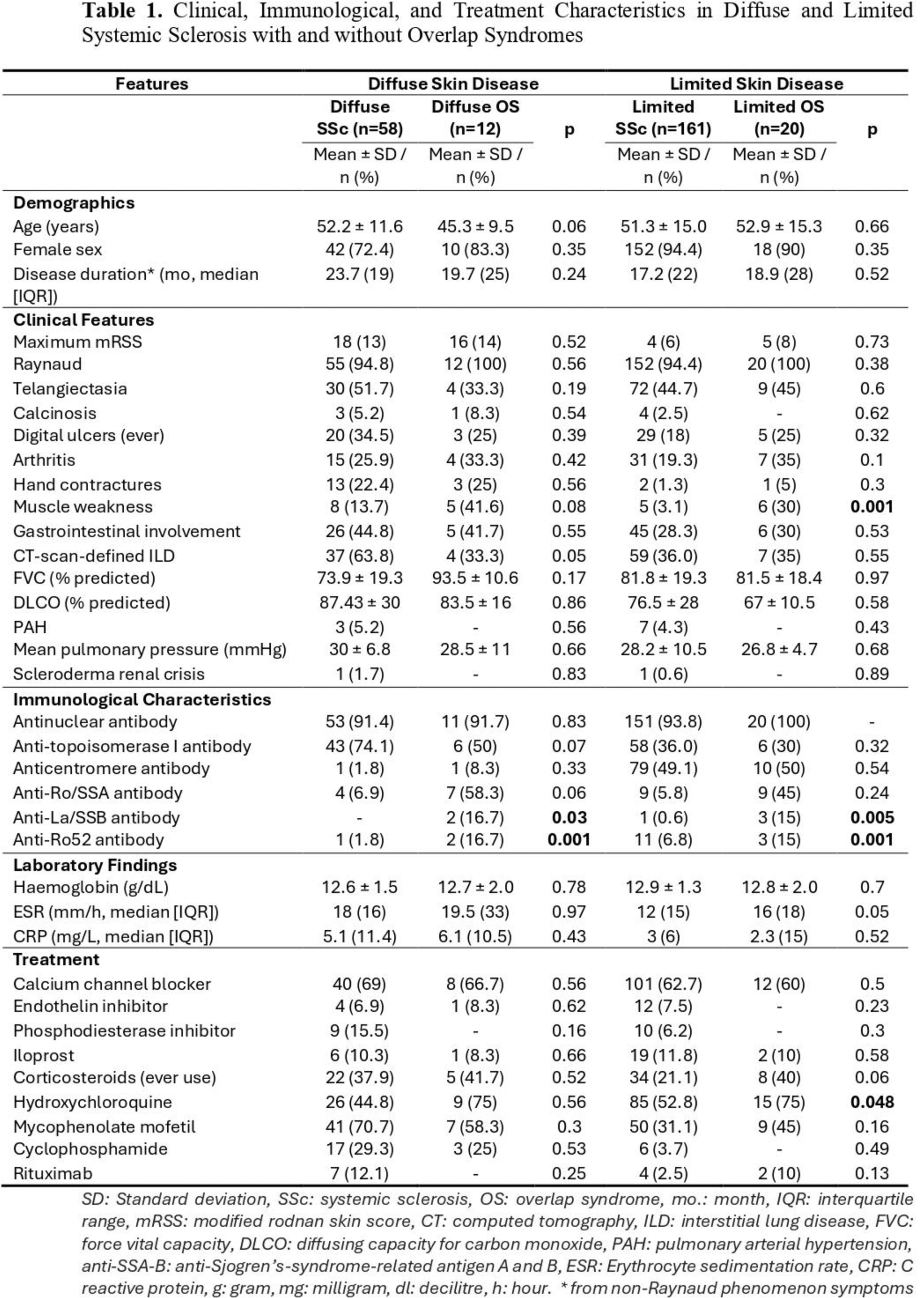
Results: Thirty-two patients had SSc-overlap syndrome. Among these patients, 6 patients had polymyositis (PM) 18 patients had SjD, 4 patients each had RA and SLE. Muscle weakness was significantly more prevalent in the diffuse OS group (42%) compared to the diffuse SSc group (13.7%). A similar pattern was observed in limited disease, 30% vs 3% patients with OS and limited SSc had muscle weakness (p = 0.001). Interstitial lung disease (ILD) was more common in diffuse SSc (64%) than in diffuse OS (33 %) (p = 0.05), while no significant differences were noted in the limited groups (p = 0.55). Anti-Ro/SSA antibodies were more frequent in both diffuse OS (58%) and limited OS (45%) groups compared to their respective SSc counterparts (6.9% in diffuse SSc, 5.8% in limited SSc; p = 0.001 for both). Anti-La/SSB antibodies were also more prevalent in the diffuse OS group (16.7%) compared to diffuse SSc (0%) (p = 0.03) and in the limited OS group (15%) versus limited SSc (0.6%) (p = 0.005). patients with limited OS received more frequently (75%) compared to the patients with isolated limited SSc (53%) (p = 0.048). Other treatment preferences of the physicians, including mycophenolate mofetil, glucocorticoids, and cyclophosphamide, were similar between the groups.
Conclusion: In this study, the prevalence of OS among SSc patients was 13%, consistent with previous literature [1, 2, 3]. Muscle weakness was significantly more common in OS across both diffuse and limited subtypes, whereas ILD was less frequent in diffuse OS compared to diffuse SSc. The higher prevalence of anti-Ro/SSA and anti-La/SSB antibodies in OS patients further highlights the distinct immunological features associated with overlap syndromes, potentially indicating a different underlying disease mechanism. Despite these clinical and immunological differences, OS had a limited impact on treatment preferences. We need longer follow-up period to deliniate the prognostic importance.
REFERENCES: [1] Foocharoen C, Netwijitpan S, Mahakkanukrauh A, Suwannaroj S, Nanagara R. Clinical characteristics of scleroderma overlap syndromes: comparisons with pure scleroderma. Int J Rheum Dis. 2016;19(9):913-923. doi:10.1111/1756-185X.12884.
[2] Jantarat A, Muangchan C. Epidemiology and clinical characteristics of systemic sclerosis overlap syndrome (SSc-OS), and the factors significantly associated with SSc-OS in Thai patients with systemic sclerosis. Mod Rheumatol. 2022;32(5):899-907. doi:10.1093/mr/roab079.
[3] Pakozdi A, Nihtyanova S, Moinzadeh P, Ong VH, Black CM, Denton CP. Clinical and serological hallmarks of systemic sclerosis overlap syndromes. J Rheumatol. 2011;38(11):2406-2409. doi:10.3899/jrheum.101248.
Acknowledgements: NIL.
Disclosure of Interests: None declared.
© The Authors 2025. This abstract is an open access article published in Annals of Rheumatic Diseases under the CC BY-NC-ND license (