

Background: Several studies in systemic lupus erythematosus (SLE) have suggested that males may experience greater damage accrual compared to females. However, this has not been adequately explored in cohorts focused specifically on lupus nephritis (LN), particularly with the separate consideration of renal and extra-renal damage.
Objectives: We aimed to investigate biologic sex-based differences in the accrual of both extra-renal and renal damage in a cohort of LN patients.
Methods: This retrospective study included patients with systemic lupus erythematosus (SLE) from an observational cohort who developed LN at or after clinic entry. Outcomes of extra-renal and renal damage were assessed. For extra-renal damage, the Systemic Lupus International Collaborating Clinics (SLICC)/American College of Rheumatology (ACR) Damage Index (SDI) was used, excluding the renal item (non-renal SDI). For renal damage, a composite measure was used, defined as a sustained ≥ 30% decline in estimated glomerular filtration rate (eGFR) or end-stage kidney disease (ESKD). Univariable and multivariable Fine-Gray subdistribution hazard models were utilized to identify baseline features associated with the first outcome, an increase in non-renal SDI by ≥1, employing death as used as a competing risk. The models were adjusted for age, hypertension, baseline SDI, glucocorticoid dose, and ‘LN before 2005 vs. 2005 or after’ to account for the calendar effect; mycophenolate mofetil became available in our cohort after the year 2005 and it was around that time when a more glucocorticoid-conservative approach was followed. Likewise, univariable and multivariable Fine-Gray subdistribution hazard models were then utilized to identify baseline features associated with the composite outcome employing death as a competing risk. The models were adjusted for baseline serum creatinine level and calendar effect.
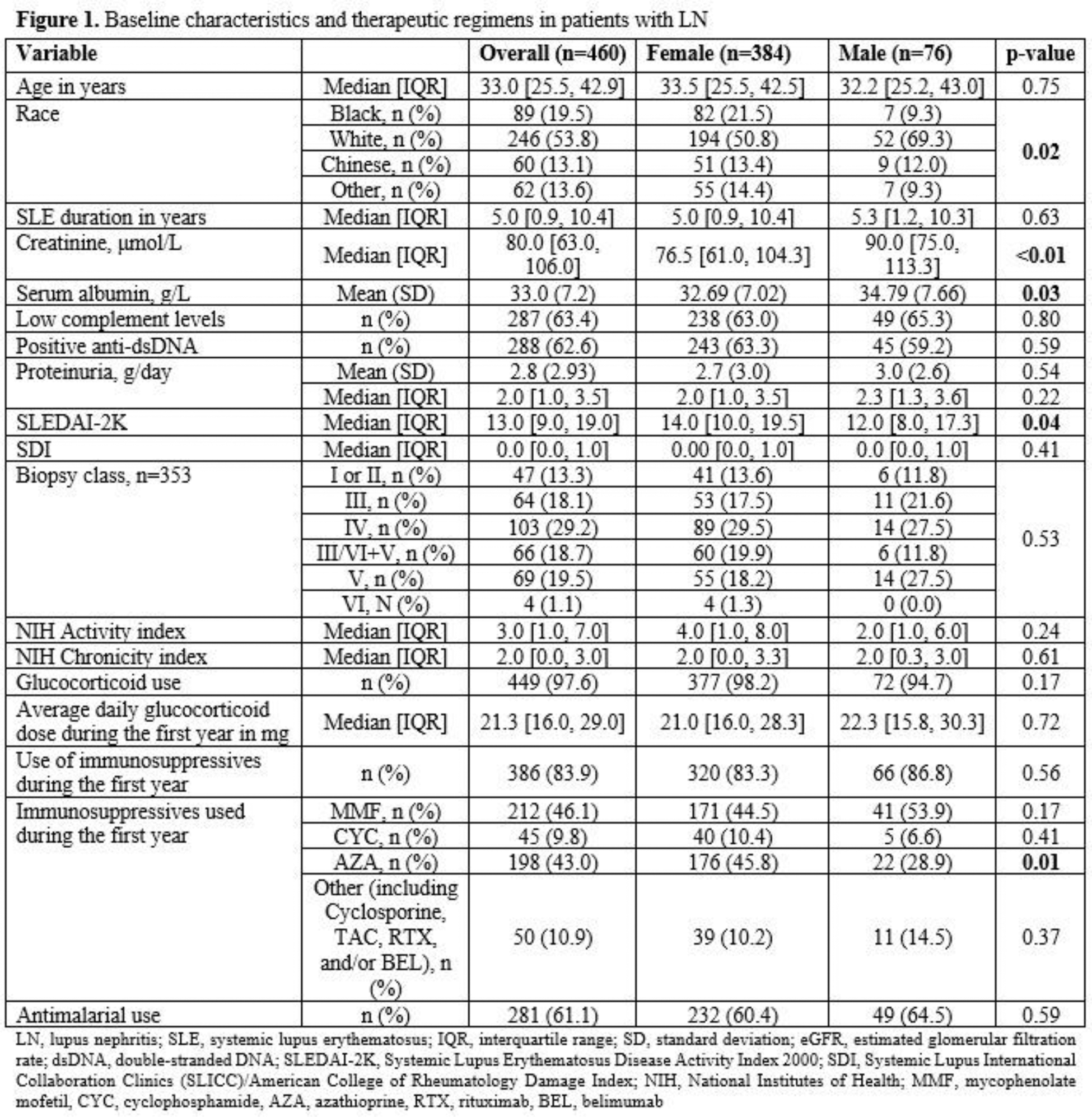
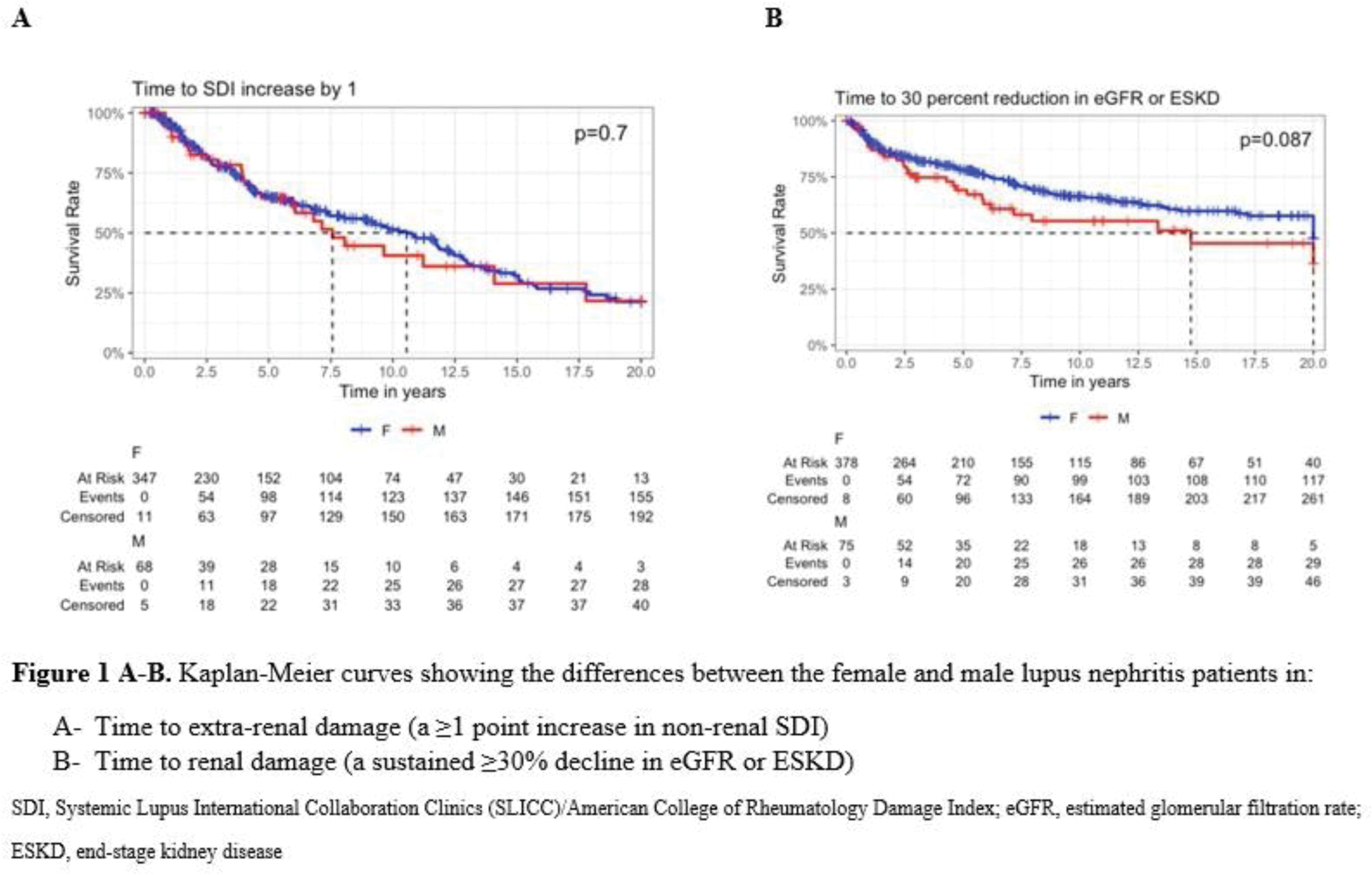
Results: The LN cohort included 460 patients, with a predominance of females (83.5%) and a median age of 33 years. Female patients were more likely to be Black, and there were no significant differences in baseline SDI or renal histology between males and females (Table 1). Over a median follow-up of 8.6 years [IQR: 4.1, 14.9], 45% of patients accrued extra-renal damage, while 32% experienced renal damage. Notably, the median time to extra-renal damage was numerically shorter than that for renal damage (4.1 [1.6, 8.7] vs. 5.5 [1.7, 11.3] years). No significant differences in the accrual of either extra-renal or renal damage were observed between males and females, and the time to these outcomes was not statistically different between sexes (Figure 1). The most common SDI items identified in the 188 patients who accrued extra-renal damage were ocular (36.7%), diabetes mellitus (15.4%), skin (13.8%), musculoskeletal (9.6%), and neurologic (8.5%). Aside from neurologic damage, which was more prevalent in males (20.7% [6/29] in males vs. 6.2% [10/159] in females, p = 0.04), no significant differences based on sex were found. When examining the SDI organ items, peripheral neuropathy was more frequent in males (13.8 [4/29] % vs. 2.5% [4/159], p = 0.02). Multivariate analyses revealed that male sex was not associated with greater damage accrual, either extra-renal (HR 1.04, 95% CI 0.71–1.54) or renal (HR 1.27, 95% CI 0.69–2.32).
Conclusion: Extra-renal and renal damage accrual are common in patients with LN but do not appear to occur more rapidly in males. We suggest that optimizing treatment protocols through multitargeted therapy and reducing glucocorticoid exposure may improve long-term outcomes.
REFERENCES: NIL.
Acknowledgements: NIL.
Disclosure of Interests: Fadi Kharouf: None declared, Pankti Mehta: None declared, Ali Alhadri: None declared, Qixuan Li: None declared, Laura Whittall Garcia: None declared, Dafna D. Gladman AstraZeneca, Abbvie, Amgen, BMS, Eli Lilly, GSK, Janssen, Novartis, Pfizer, UCB, Abbvie, Amgen, Eli Lilly, Janssen, Novartis, Pfizzer, UCB, Zahi Touma: None declared.
© The Authors 2025. This abstract is an open access article published in Annals of Rheumatic Diseases under the CC BY-NC-ND license (