

Background: Anti-ribosomal P antibodies (aRibP) are highly specific markers for systemic lupus erythematosus (SLE), particularly in cases involving renal, psychiatric, or hepatic manifestations [1, 2]. Their role as prognostic markers has also been noted, with associations to lupus nephritis linked to a favorable prognosis [3]. However, isolated positivity for aRibP is not widely documented in the literature, raising questions about its clinical relevance and utility in the diagnosis and monitoring of autoimmune diseases.
Objectives: The aim of the study was to describe the clinical and laboratory characteristics of patients with isolated positivity for antiribosomal P antibodies (aRibP) in a cohort from a tertiary hospital’s autoimmune laboratory.
Methods: A retrospective observational study was conducted on samples testing positive for aRibP in the autoimmune laboratory of the Hospital Universitario Fundación Jiménez Díaz between December 28, 2018, and May 29, 2024. The positivity criterion for aRibP included identifying a compatible pattern through indirect immunofluorescence on HEp-2 cells (AC-19) and confirmation using at least two solid-phase immunoassay techniques: immunoblot (Euroimmun®/DTEK®) and either Biorad-Bioplex® or ELiA-Thermofisher. Patients with concurrent antibodies—anti-SSA/Ro52, anti-SSA/Ro60, anti-SSB/La, anti-CENPB, anti-Sm, anti-U1RNP, anti-dsDNA, antinucleosomes, and antihistones—were excluded. A descriptive review of the medical records of these patients was also performed to identify their characteristics, establish the underlying pathologies and determine the associated manifestations.
Results: Out of 404,599 aRibP determinations, 172 tested positive according to the study’s inclusion criteria. Of these, 141 samples were associated with other antibodies, while 31 represented isolated aRibP positivity. These 31 positive samples corresponded to 16 unique patients, whose medical records were reviewed. The clinical findings are summarized in Table 1.
Clinical Analysis of the 16 Patients Included in the Study
| Group | Cases, n (%) | Sex women, n (%) | Age, years median (range) | |
|---|---|---|---|---|
| Autoinmune diseases | ||||
| SLE | 6 (37.5) | 3 (37.5) | 49 (49-65) | |
| CLE | 1 (6.25) | 1 (12.5) | 44 | |
| ATP | 1 (6.25) | 1 (12.5) | 29 | |
| Autoinmune hypotiroidism | 1 (6.25) | 1 (12.5) | 69 | |
| IPAF | 1 (6.25) | 0 | 76 | |
| Inflammatory diseases | ||||
| Pneumonia | 1 (6.25) | 0 | 49 | |
| Mixed cryoglobulinemia due to HCV | 2 (12.5) | 1 (12.5) | 76.5 (76-77) | |
| Others | ||||
| Pancreatic cancer | 1 (6.25) | 1 (12.5) | 60 | |
| Without disease | 3 (18.75) | 0 | 57 (49-57) | |
| Total | 16 (100) | 8 (12.5) | 57 (29-76.5) | |
Systemic lupus erythematosus (SLE); Cutaneous lupus erythematosus (CLE); IPAF (Interstitial pneumonia with autoimmune features); Autoimmune thrombocytopenic purpura (ATP); Hepatitis C virus (HCV)
Patients without disease were defined as those without clinical evidence of inflammatory or autoimmune disease after a median follow-up of 14.5 months (range: 7–143 months). The clinical manifestations of SLE in the six patients with isolated aRibP were as follows: Four had cutaneous manifestations, three had arthralgia/arthritis, one had lupus nephritis, one had central nervous system involvement with lupus psychosis and generalized tonic-clonic seizures, one had lymphopenia, and another had neutropenia. aRibP levels fluctuated without any correlation to clinical relapses in the four patients in whom these antibodies were assessed (Figure 1).
Evolution of aRibP levels by ELiA and BP in patients with SLE
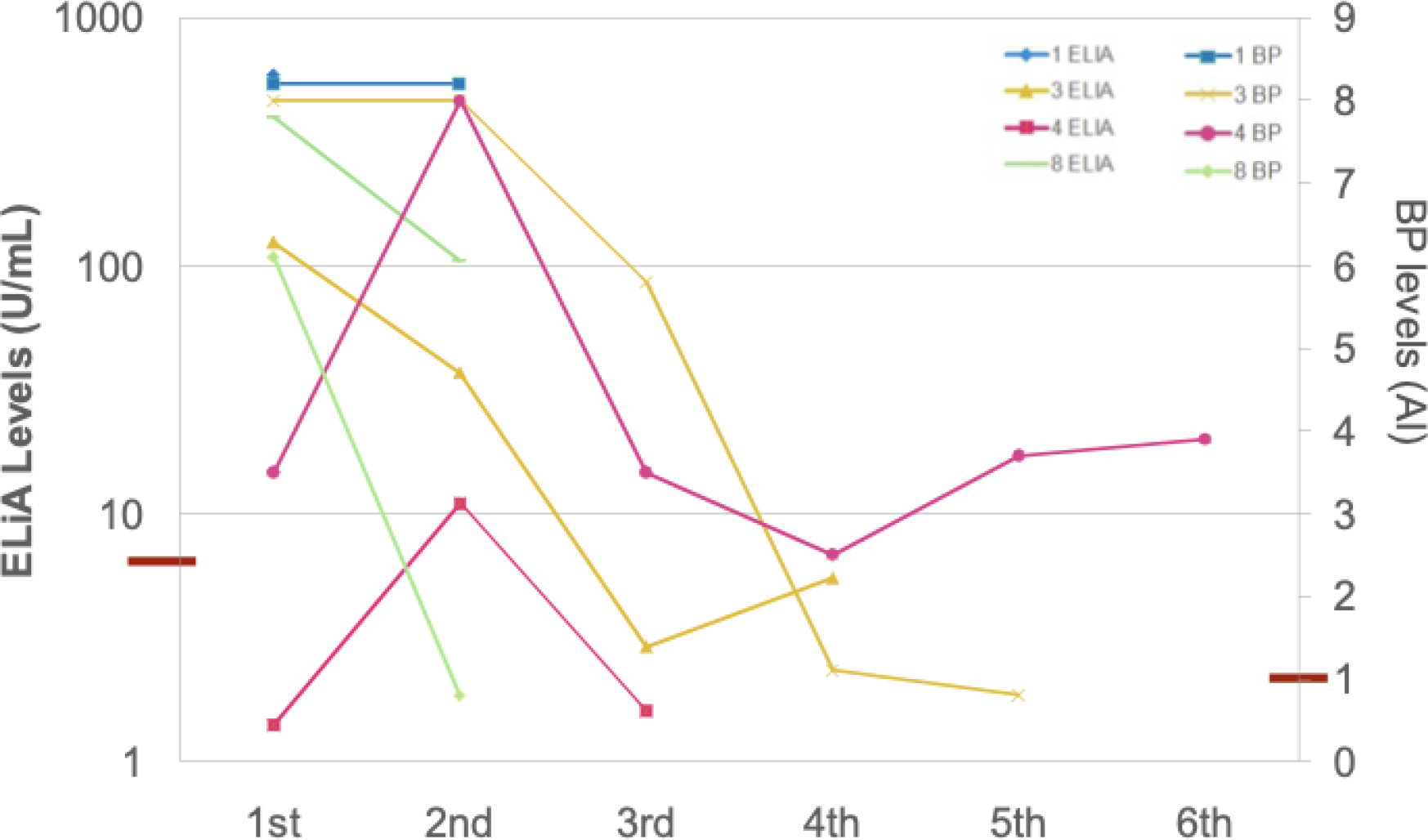
Conclusion: The isolated presence of aRibP is infrequent, and its clinical relevance remains unclear, as it is predominantly found in association with other antibodies. Most patients with isolated aRibP did not present systemic autoimmune diseases during the follow-up period, except for SLE. In this cohort, only one case of lupus psychosis with generalized tonic-clonic seizures was observed, and no cases of hepatitis were documented. Although aRibP levels fluctuated in some patients, no clear relationship with clinical relapses in SLE was identified. The sample size does not allow for definitive conclusions regarding the clinical utility of aRibP monitoring. Further studies are required to evaluate the long-term behavior of isolated aRibP and its potential utility as a follow-up marker.
REFERENCES: [1] Hirohata, S. (2011). Anti-ribosomal P antibodies and lupus nephritis. Clinical And Experimental Nephrology, 15(4), 471-477.
[2] Zhang, W., & Reichlin, M. (2004). Production and characterization of a human monoclonal anti-idiotype to anti-ribosomal P antibodies. Clinical Immunology, 114(2), 130-136.
[3] Sarfaraz, S., Anis, S., Ahmed, E., & Muzaffar, R. (2018). Clinical Significance of Anti-Ribosomal P Protein Antibodies in Patients with Lupus Nephritis. Reviews On Recent Clinical Trials, 13(4), 281-286.
Acknowledgements: NIL.
Disclosure of Interests: None declared.
© The Authors 2025. This abstract is an open access article published in Annals of Rheumatic Diseases under the CC BY-NC-ND license (