

Background: Dry eye syndrome (DES) and Sjögren’s syndrome (SJS) are debilitating conditions characterized by tear film instability, ocular surface damage, and reduced quality of life. Current pharmacologic treatments, including hydroxychloroquine for SJS, often entail significant side effects, prompting the need for safer and more effective alternatives. Acupuncture is a traditional therapy that may enhance tear production and alleviate ocular symptoms by regulating neural and vascular functions. However, high-quality clinical trials validating its efficacy and safety are limited.
Objectives: The ACUDES trial aimed to evaluate the efficacy and safety of acupuncture at GB20 (Fengchi) and GB20 combined with BL2 (Cuanzhu) in improving tear production and alleviating ocular dryness in patients with DES and SJS.
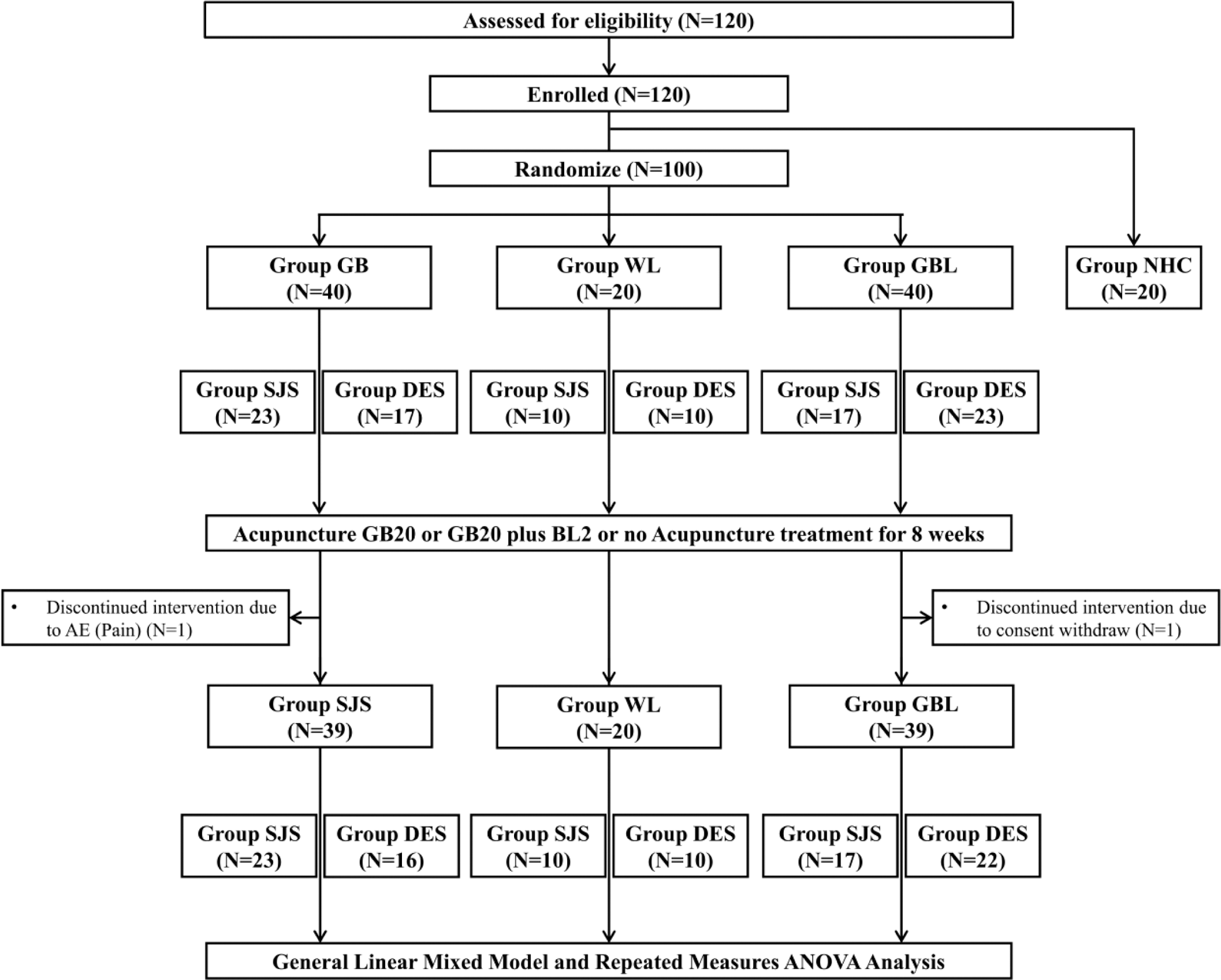
Methods: This phase-2 single-blind randomized controlled trial was conducted between October 2022 and January 2024 at Taipei Veterans General Hospital, Taiwan. A total of 100 patients, including 50 with DES and 50 with SJS, were randomly assigned to three groups: GB (acupuncture at GB20), GBL (acupuncture at GB20 and BL2), and waiting list (WL) control (Figure 1). Twenty healthy controls (NHC) were included for baseline comparison. Participants in the GB and GBL groups received acupuncture treatments twice weekly for 8 weeks. Each session lasted 20 minutes. The WL group did not receive acupuncture but continued with conventional care. Primary outcomes were Schirmer’s test and the Ocular Surface Disease Index (OSDI). Secondary outcomes included the EULAR Sjögren’s Syndrome Patient Reported Index, Tear Break-Up Time, and artificial tear usage. Safety was monitored through participant reports of adverse events, including pain, bruising, and numbness. All assessments were conducted at baseline, immediately after the first session, at 4 weeks, and at 8 weeks. Statistical analysis included repeated measures ANOVA and Tukey’s HSD for post-hoc comparisons. A p-value < 0.05 was considered significant.
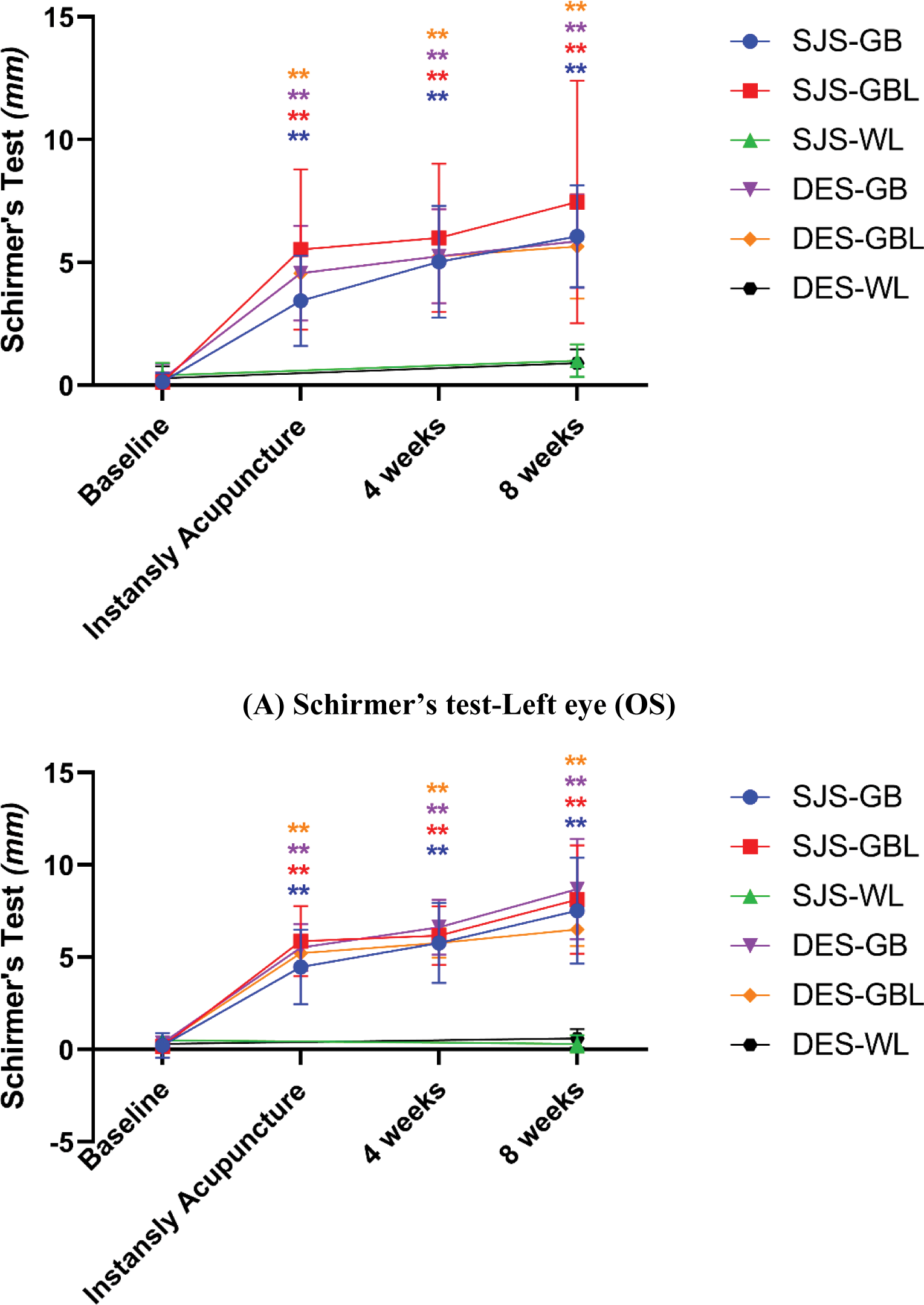
Results: Among the 120 participants (92.5% female; mean age 55.8±11.8 years), baseline demographic and clinical characteristics were comparable across groups. For Schirmer’s test (Figure 2), DES participants in the GB group showed significant improvements in tear production, with OS values improving from 0.11±0.32 mm at baseline to 7.18±4.39 mm at 8 weeks (p < 0.001), while OD values increased from 0.50±0.86 mm to 8.65±4.94 mm (p < 0.001). SJS participants in the GB group showed OS values improving from 0.13±0.34 mm to 6.44±2.09 mm (p < 0.001), and OD values from 0.09±0.29 mm to 7.50±2.91 mm (p < 0.001). In the GBL group, DES participants improved OS values from 0.26±0.62 mm to 5.86±1.91 mm (p < 0.001), and OD values from 0.30±0.56 mm to 6.50±2.06 mm (p < 0.001). SJS participants in the GBL group improved OS values from 0.12±0.33 mm to 7.47±4.94 mm (p < 0.001), and OD values from 0.18±0.53 mm to 8.12±5.73 mm (p < 0.001). In the WL group, DES participants showed minimal changes, with OS values increasing from 0.33±0.47 mm to 0.89±0.57 mm and OD values from 0.33±0.45 mm to 0.68±0.67 mm at 8 weeks. For SJS participants in the WL group, OS values rose from 0.36±0.48 mm to 0.99±0.60 mm, and OD values remained stable, increasing from 0.45±0.50 mm to 0.68±0.67 mm. For OSDI, DES participants in the GB group improved significantly, with scores decreasing from 60.83±23.30 at baseline to 33.66±15.31 at 8 weeks (p < 0.001). SJS participants in the GB group showed similar improvement, with scores decreasing from 51.51±27.04 to 34.47±20.86 (p < 0.001). In the GBL group, DES participants improved from 55.94±21.68 to 35.18±17.89 (p < 0.001), and SJS participants from 57.43±18.52 to 36.39±22.66 (p < 0.001). In the WL group, DES participants exhibited slight increases in scores from 59.15±24.01 to 60.99±24.65, and SJS participants showed marginal changes from 39.51±20.37 to 40.34±20.73. For artificial tear usage, DES participants in the GB group showed reductions from 4.62±4.49 times/day at baseline to 1.06±1.29 times/day at 8 weeks (p < 0.001), and SJS participants reduced usage from 6.65±6.34 times/day to 1.04±1.39 times/day (p < 0.001). In the GBL group, DES participants reduced usage from 5.65±6.92 times/day to 1.44±1.41 times/day (p < 0.001), and SJS participants from 4.29±1.45 times/day to 0.88±0.69 times/day (p < 0.001). Minimal changes were noted in the WL group. Adverse events were mild and transient, with the most common being pain and bruising. No severe adverse events were reported.
Participant Enrollment and Group Allocation of ACUDES trial.
The primary outcome of Schirmer’s test in the ACUDES trial within the Sjögren’s Syndrome group (SJS), and Dry eye syndrome group (DES). (A) Schirmer’s test OS (left eye), and (B) Schirmer’s test OD (right eye). GB group: received bilateral acupuncture at GB20; GBL group: received bilateral acupuncture at both GB20 and BL2; WL (Waiting list) group: did not receive any acupuncture but continued with conventional therapy
Conclusion: Acupuncture at GB20 and GB20 plus BL2 is a safe and effective intervention for improving ocular dryness in patients with DES and SJS. It offers a viable non-pharmacologic alternative, especially for those seeking to avoid the side effects of conventional treatments. Larger, multicenter trials are recommended to confirm these results and evaluate the long-term benefits of acupuncture for dry eye management.
REFERENCES: NIL.
Acknowledgements: This study was supported by the Center for Traditional Medicine, Taipei Veterans General Hospital, Taipei, Taiwan (V108B-031, V109B-034, V112C-190, and V113C-087), National Yang Ming Chiao Tung University, Taipei, Taiwan, and National Science and Technology Council, Taipei, Taiwan (NSTC-111-2320-B-A49A-501 -MY2 and NSTC-113-2320-B-A49-029). We would like to thank the following researchers for their help in the enrollment of subjects and data analysis: Dr. Yin-Chun Liao, Mr. Shu-Wei Hung, and Mr. Jin-An Chang from Taipei Veterans General Hospital, Taipei, Taiwan, and National Yang Ming Chiao Tung University, Taipei, Taiwan, respectively.
Disclosure of Interests: None declared.
© The Authors 2025. This abstract is an open access article published in Annals of Rheumatic Diseases under the CC BY-NC-ND license (