

Background: A majority of patients with eosinophilic granulomatosis with polyangiitis EGPA present with severe eosinophilic asthma and nasal polyposis, which can lead to misdiagnosis and delays in appropriate treatment. Consequently, distinguishing EGPA from similar conditions is crucial. Current unmet needs include standardized diagnostic criteria and reliable biomarkers to differentiate EGPA from other type 2 inflammatory diseases, such as severe eosinophilic asthma and chronic rhinosinusitis with nasal polyps (CRSwNP). Circulating anti-Pentraxin 3 (PTX3) autoantibodies have been identified in autoimmune conditions such as systemic lupus erythematosus, where they may exert anti-inflammatory effects. Recent studies have shown a higher prevalence of anti-PTX3 antibodies in EGPA patients. Moreover, a distinct immunofluorescence pattern has been observed, differing from cytoplasmic and perinuclear staining, suggesting PTX3 as a potential novel ANCA antigen.
Objectives: The aim of this study is to investigate levels and prevalence of anti- PTX3 autoantibodies in the sera of patients with EGPA, severe eosinophilic asthma and CRSwNP. The objective is to identify a potential biomarker that can help distinguish severe asthma or CRSwNP patients who may be in a prodromal phase of EGPA, thereby aiding in early diagnosis and guiding diagnostic decision-making strategies.
Methods: We conducted a single-center, cross-sectional study, including unselected patients classified as EGPA, according to the 2022 American College of Rheumatology classification criteria, or severe eosinophilic asthma or CRSwNP. Anti-PTX3 levels were measured using a standardized, in-house enzyme-linked immunosorbent assay (ELISA) in sera from patients with EGPA and compared to those with severe asthma and CRSwNP. The cut-off for positive anti-PTX3 antibody detection was set at an optical density (OD) of 0.234 at 405 nm, as previously reported [1]. Liquid-phase inhibition tests were conducted to assess potential interferences. Descriptive statistics (medians, percentages, and interquartile ranges) summarized cohort characteristics. The Mann-Whitney was used for continuous variables, and the chi-square test for categorical variables.
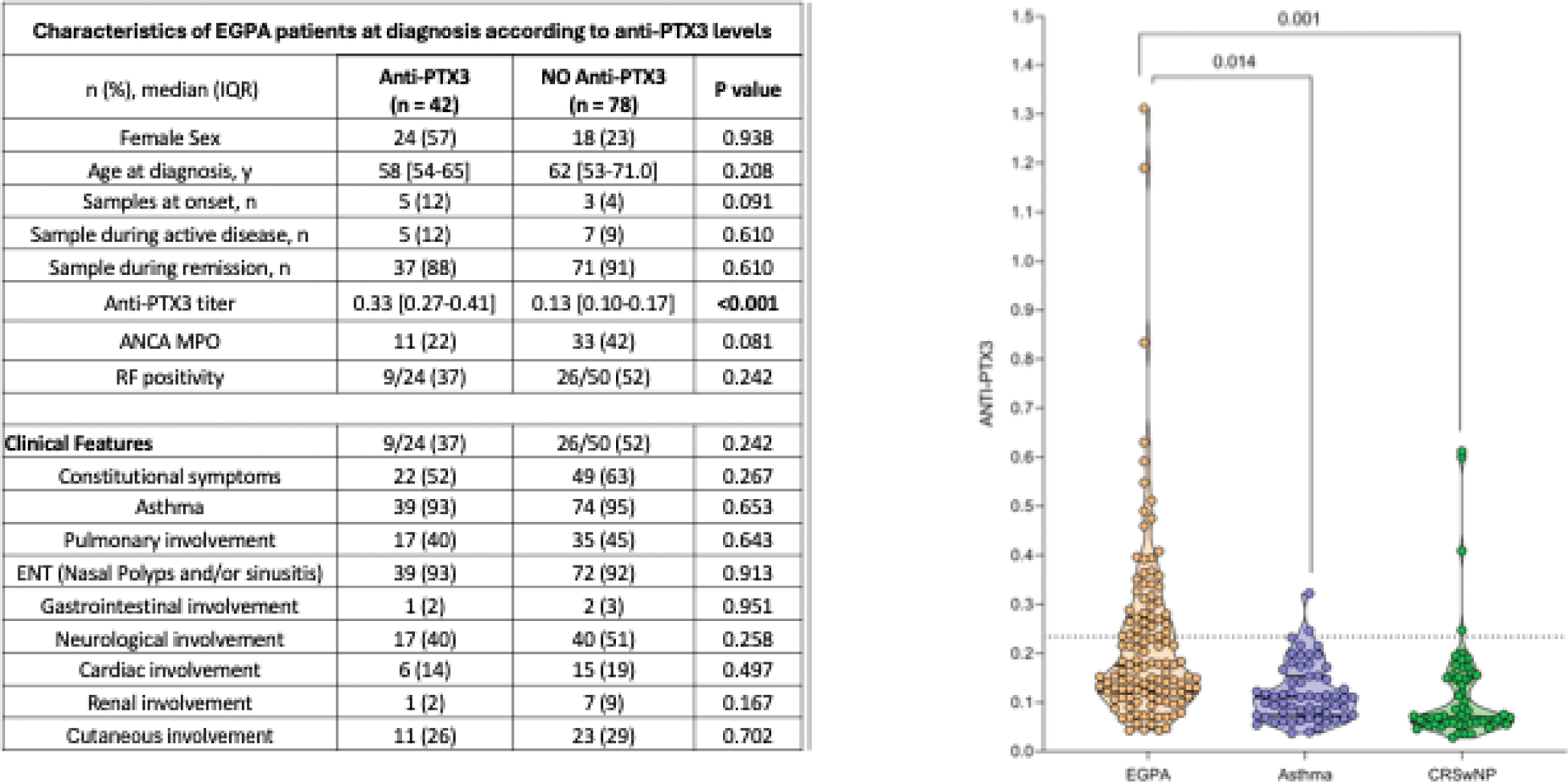
Results: A total of 120 patients diagnosed with EGPA were included, of whom 68 (56.7%) were female, with a median age of 61 years [54–69]. At the time of diagnosis, 44 (36.7%) patients were positive for ANCA, all with anti-MPO specificity. The control group consisted of patients with either eosinophilic asthma (n= 60, 41 females (68.3%), median age 59 [52-65] years) or CRSwNP (n= 63, 18 females (44.4%), median age 58 [48-67] years). Anti-PTX3 antibodies were detected in 42 (35%) out of 120 EGPA patients. The prevalence of anti-PTX3 antibodies was significantly higher in EGPA patients compared to those with asthma (42/120 35% vs 1/59 1.7%, p<0.001) and with CRSwNP (41/120 35% vs 3/63 4.8%, p<0.001), with p value comprehensive p < 0.001. Accordingly, median OD of anti-PTX3 resulted higher in EGPA than in asthma patients (0.14 [0.07–0.26] vs. 0.11 [0.07–0.15], p = 0.014) and CRSwNP patients (0.14 [0.07–0.26] vs. 0.07 [0.06–0.15], p = 0.001). The frequency of anti-PTX3 antibodies did not differ significantly based on ANCA status (25% in ANCA-positive patients vs. 40.8% in ANCA-negative patients, p = 0.801). No significant differences in anti-PTX3 antibody levels were observed based on clinical features at the time of diagnosis.
Conclusion: Anti-PTX3 autoantibodies represent a promising novel biomarker for EGPA. Their prevalence is significantly higher in EGPA compared to other type 2 inflammatory diseases and may serve as a valuable tool to aid early diagnosis and guide treatment decision in patients with eosinophilic asthma or CRSwNP, suspected of progressing to EGPA.
REFERENCES: [1] Padoan et al. Journal of Autoimmunity, 2021.
Acknowledgements: NIL.
Disclosure of Interests: None declared.
© The Authors 2025. This abstract is an open access article published in Annals of Rheumatic Diseases under the CC BY-NC-ND license (