

Background: An effective doctor-patient relationship is crucial in the management of systemic lupus erythematosus (SLE) [1, 2] and has the potential to improve adherence and impact treatment outcomes [3]. However, the current state of this critical therapeutic component in SLE management remains underexplored. Differences from Europe to other geographies and, indeed, within Europe, have not been addressed so far. Understanding these dynamics can help both physicians and patients better work towards improved outcomes.
Objectives: To explore how the doctor-patient relationship is perceived among European lupus patients, with a focus on trust, shared decision-making, treatment adherence, and satisfaction with care.
Methods: As part of the Lupus Europe Living with Lupus 2024 programme, respondents were asked to assess factors such as trust, treatment adherence, shared decision-making, and satisfaction with care. Descriptive statistics and correlation analyses were employed to identify key trends and associations.
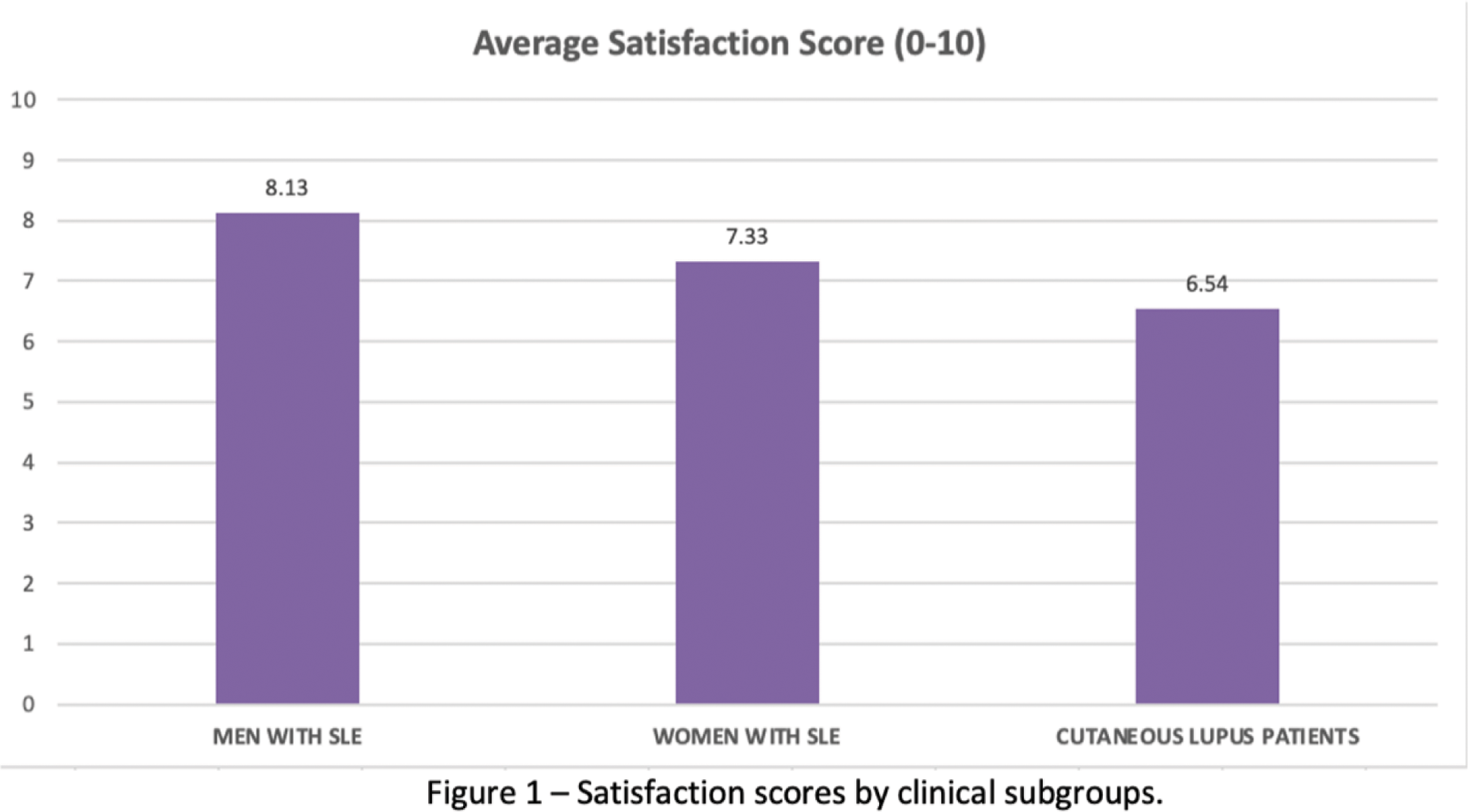
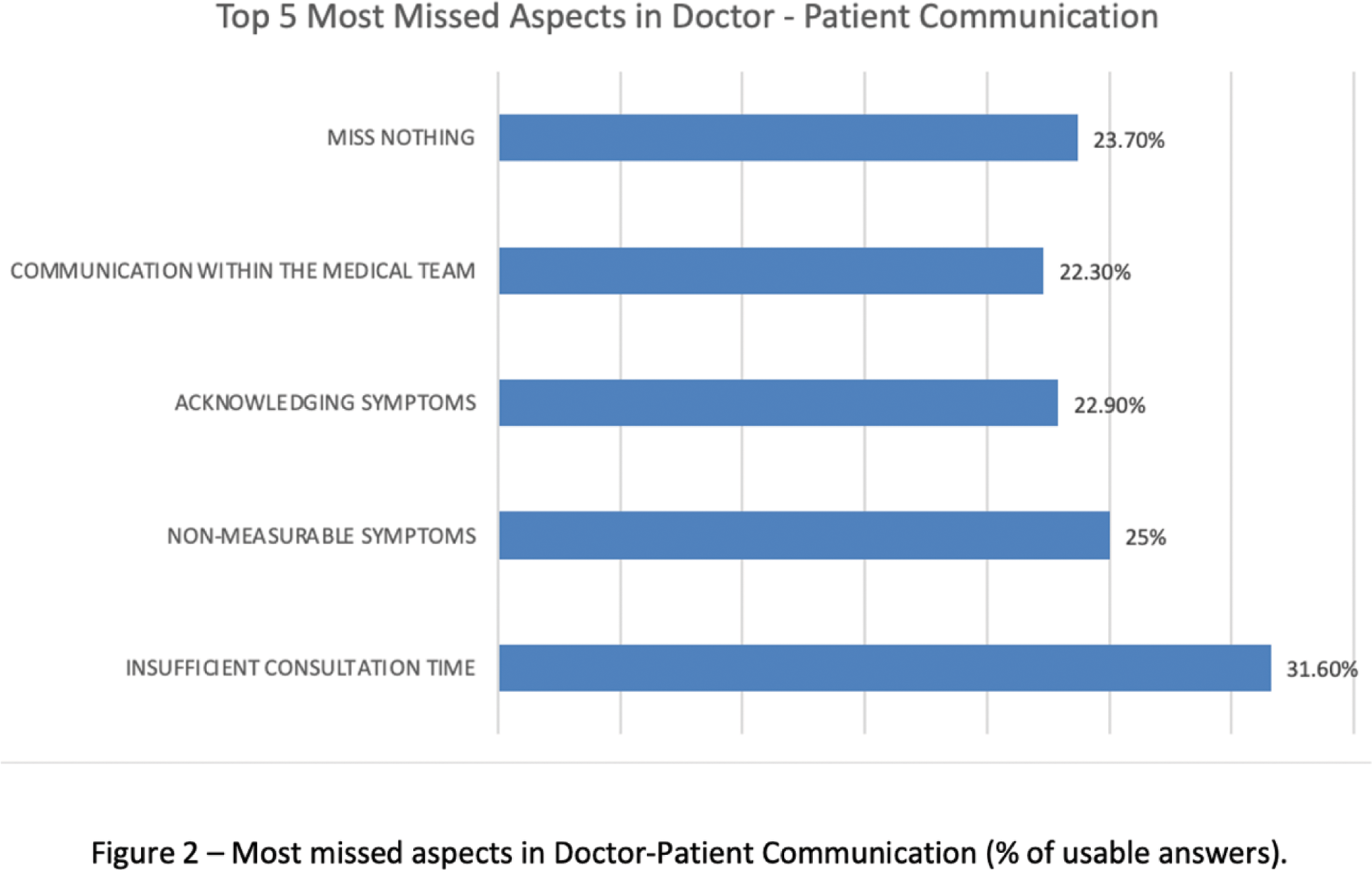
Results: Responses from 3834 European SLE patients who completed the relevant sections of the questionnaire were included in this analysis. The majority (92,5%, n=3650) identified as women, 148 as men, 36 did not respond or preferred not to say. Mean age was 45,7 years (±12,5). On a scale from 0 (fully unsatisfied) to 10 (fully satisfied), patients scored overall satisfaction with the care provided by their team at an average 7.33 (±2.39). Men reported higher satisfaction than women (8.13 vs. 7.33, p<0.001), those with cutaneous lupus were least satisfied (6.54, p<0.001). Overall satisfaction strongly correlated (r=0.72) with “having a trustful relationship with my doctor” and moderately correlated with the “doctor taking into account my opinion when managing my treatment” (r=0.65) and “taking into account my psychological wellbeing” (r=0.61). Interestingly, there was no correlation between this overall satisfaction and saying, “the truth, all the truth and only the truth to my HCP with regards to my adherence to my treatment”. Trust in the doctor-patient relationship showed a strong polarisation, 47.4% (n=1812) rated it 9 or 10 (on a 1 to 10 scale), but 21.4% (n=818) scored it below 5 (mean 7.56, SD 2.58). 737 respondents (26.4%) scored 5 or less for “the doctor takes into account my opinion when managing my treatment”, 979 (26.4%) scored 5 or less for “I am a key contributor to shared decision making about my treatment management”. 702 (18.9%) scored 5 or less for “I have an active role in controlling my disease”. 730 participants (19.7%) scored below 5 for “I can share all my problems with my doctor” and 1140 respondents (30.7%) scored below 5 for “my doctor takes into account my psychological well-being”. Only 242 respondents (6.6%) admit they do not say “the truth, all the truth and only the truth to my HCP with regards to my adherence to my treatment”. This surprisingly low number highlights the difficulty of obtaining, even on an anonymous survey, reliable information on this (over-) sensitive matter. A third (31.6%) of patients identified insufficient consultation time as one of the top 5 things they “most miss” in their patient/doctor communication, followed by lack of consideration for non-measurable symptoms (25.0%), acknowledging the symptoms patients mention (22.9%) and communication within the medical team (22.3%). Almost 1 out of 4 (23.7%) of respondents stated they miss nothing in patient/doctor interactions, and this number went up to 36.7% for men.
Conclusion: The 2024 Living with Lupus survey programme provides a nuanced understanding of the doctor-patient relationship from the perspective of thousands of European lupus patients. While overall satisfaction with care is relatively high, there exist disparities in satisfaction based on specific aspects of the doctor-patient relationship. Trust and shared decision-making emerge as strongly associated with patient satisfaction. The data also reveal actionable areas for targeted improvement. A significant proportion of respondents scored trust, shared decision making, the doctor taking into account their opinion when managing treatment, having an active role in controlling their disease, being able to share all problems with the doctor below 5 on a 1 to 10 scale. Respondents also identified other actionable areas for improvement, including acknowledging and addressing non-measurable symptoms reported by patients, acknowledging the symptoms patients mention and improving communication within the medical team. These findings highlight tangible opportunities for improvement of the patient-doctor relationship. Prioritising these patient-identified needs, can enhance communication and could result in improved care.
REFERENCES: [1] Beusterien K, Bell JA, Grinspan J, Utset TO, Kan H, Narayanan S. (2013) Physician-patient interactions and outcomes in systemic lupus erythematosus (SLE): a conceptual model. Lupus . 22(10):1038-45. doi: 10.1177/0961203313499958. PMID: 23963432.
[2] Yelin E, Yazdany J, Trupin L. (2017) Relationship Between Process of Care and a Subsequent Increase in Damage in Systemic Lupus Erythematosus. Arthritis Care Res (Hoboken ).; 69(6):927-932. doi: 10.1002/acr.22977. Epub 2017 May 9. PMID: 27477567; PMCID: PMC5285489.
[3] Sun K, Eudy AM, Criscione-Schreiber LG, Sadun RE, Rogers JL, Doss J, Corneli AL, Bosworth HB, Clowse MEB (2021). Racial Differences in Patient-provider Communication, Patient Self-efficacy, and Their Associations With Systemic Lupus Erythematosus-related Damage: A Cross-sectional Survey. J Rheumatol. 48(7):1022-1028. doi: 10.3899/jrheum.200682. Epub 2020 Sep 1. PMID: 33259332; PMCID: PMC10698393.
Acknowledgements: NIL.
Disclosure of Interests: Alain Cornet: None declared, Jeanette Andersen: None declared, Elisabeth Elfriede Wijsma: None declared, Aldevina Sturiene: None declared, Andri Spanou Nicolaou: None declared, Daniel Guimarães de Oliveira GlaxoSmithKline, AstraZeneca.
© The Authors 2025. This abstract is an open access article published in Annals of Rheumatic Diseases under the CC BY-NC-ND license (